Winkelwagen
U heeft geen artikelen in uw winkelwagen
Das nummuläre Ekzem wird oft mit kortisonhaltigen Salben behandelt, die entzündungshemmend wirken. Sind die betroffenen Hautbereiche mit Bakterien infiziert, verschreiben Ärztinnen und Ärzte zudem ein gegen die Bakterien gerichtetes Antibiotikum.
Darüber hinaus kommen manchmal Antihistaminika zum Einsatz, um insbesondere in der Nacht Juckreiz zu mildern und Schlafstörungen zu vermeiden. Antihistaminika wirken gegen allergische Reaktionen.
Grundsätzlich ist es wichtig die Haut zu schützen und schonend zu pflegen. Es empfiehlt sich beispielsweise:
The management of nummular dermatitis focuses on restoring the natural skin barrier and avoiding behaviors that dry and irritate the skin.[14]
General Measures
Topical Therapies
High- or ultrahigh potency (classes I-III) topical corticosteroids applied directly to affected skin 1 to 2 times daily help decrease inflammation and pruritus. Topical calcineurin inhibitors (tacrolimus, pimecrolimus) may be used as steroid-sparing topical agents. A typical alternating schedule includes topical corticosteroids on weekdays and topical calcineurin inhibitors on weekends. For isolated recalcitrant lesions, intralesional triamcinolone may be a treatment option (0.5-1 mL of 4-5 mg/mL triamcinolone per lesion).
Phototherapy
For widespread disease in which topical treatment may not be feasible, narrowband UVB light therapy should be considered. Light therapy should be administered 2 to 3 times weekly, slowly titrating to the appropriate duration and desired clinical response. The therapy should be discontinued if a response is not noted after 30 treatments. In patients who respond, the frequency should be reduced to once weekly for a month, then to every other week for 2 months, as needed and tolerated. For all patients undergoing phototherapy, the potential increased risk of skin cancer should be weighed against the benefits of avoiding the use of systemic immunosuppressants in the individual patient.
Systemic Therapies
If light therapy is not available, systemic immunosuppressants and immunomodulators have been used to treat extensive recalcitrant disease, including:
Systemic corticosteroids: Oral prednisone can be initiated at 40 mg per day, with the dose reduced by 10 mg every 5 days before being discontinued. Alternatively, intramuscular triamcinolone at a dose of 40 mg can be given up to once every 3 months.
Methotrexate: A dose of 10 to 15 mg per week is an alternative therapy for patients for whom systemic corticosteroids are contraindicated or for whom the disease recurs shortly after corticosteroid discontinuation.[16]
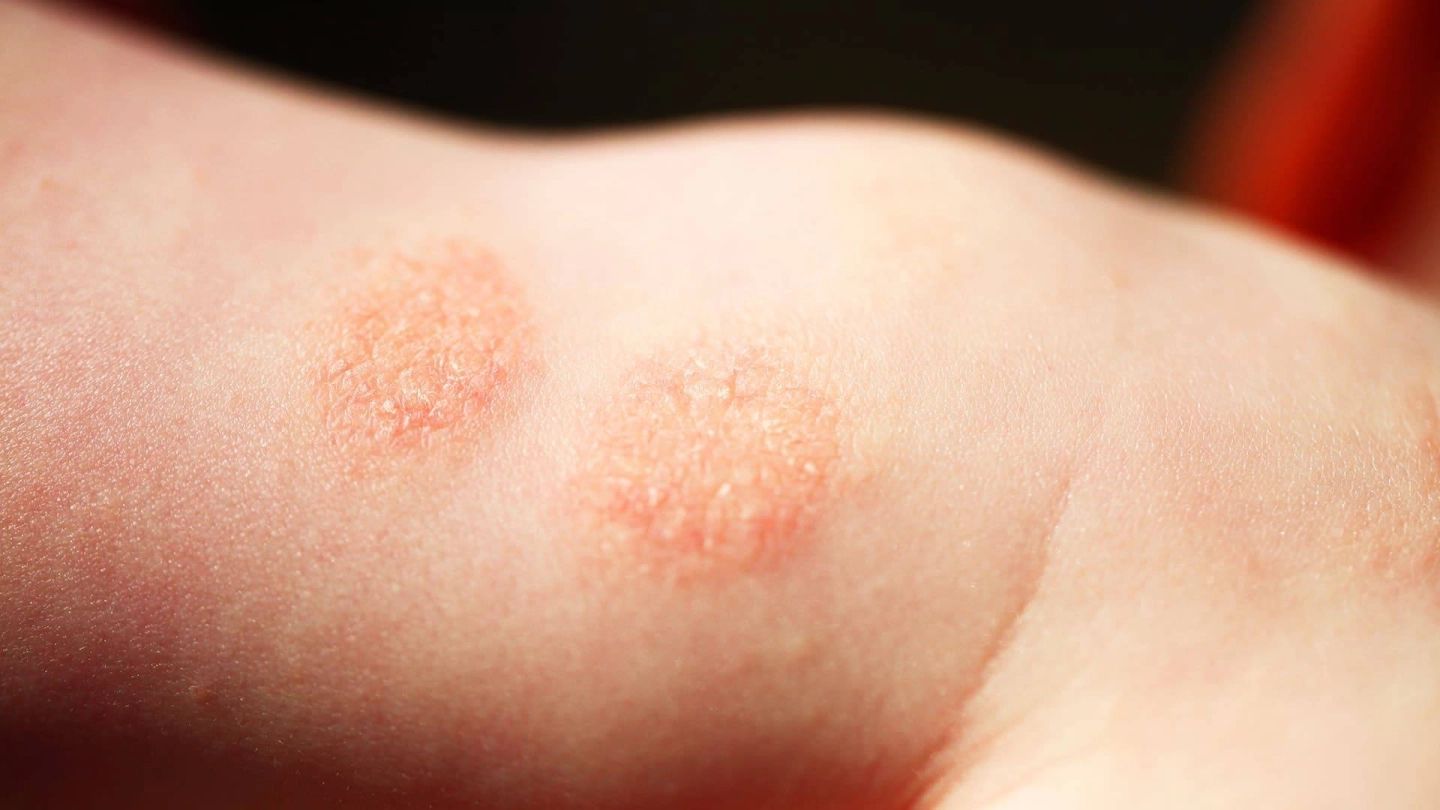
Most nummular dermatitis cases should respond to conservative measures such as gentle skincare and bland emollients used in combination with mid- to high-potency steroids. Consultation with a dermatologist should be considered in refractory, widespread, or atypical cases. Further evaluation may include skin scraping with potassium hydroxide preparation, bacterial swab for culture and sensitivities, biopsy, or patch testing, as discussed previously. If narrow-band UVB light therapy, systemic immunosuppressant, or immunomodulator is warranted, this should also be carried out under a dermatologist's supervision.
Treatment of nummular dermatitis can be optimized with an interprofessional team approach. The patient’s nurse, primary care provider, or dermatologist should monitor for therapy compliance, report any adverse effects, and relay the response to therapy to the remainder of the team. This interprofessional teamwork will enhance patient outcomes and minimize adverse reactions in caring for patients with nummular dermatitis.
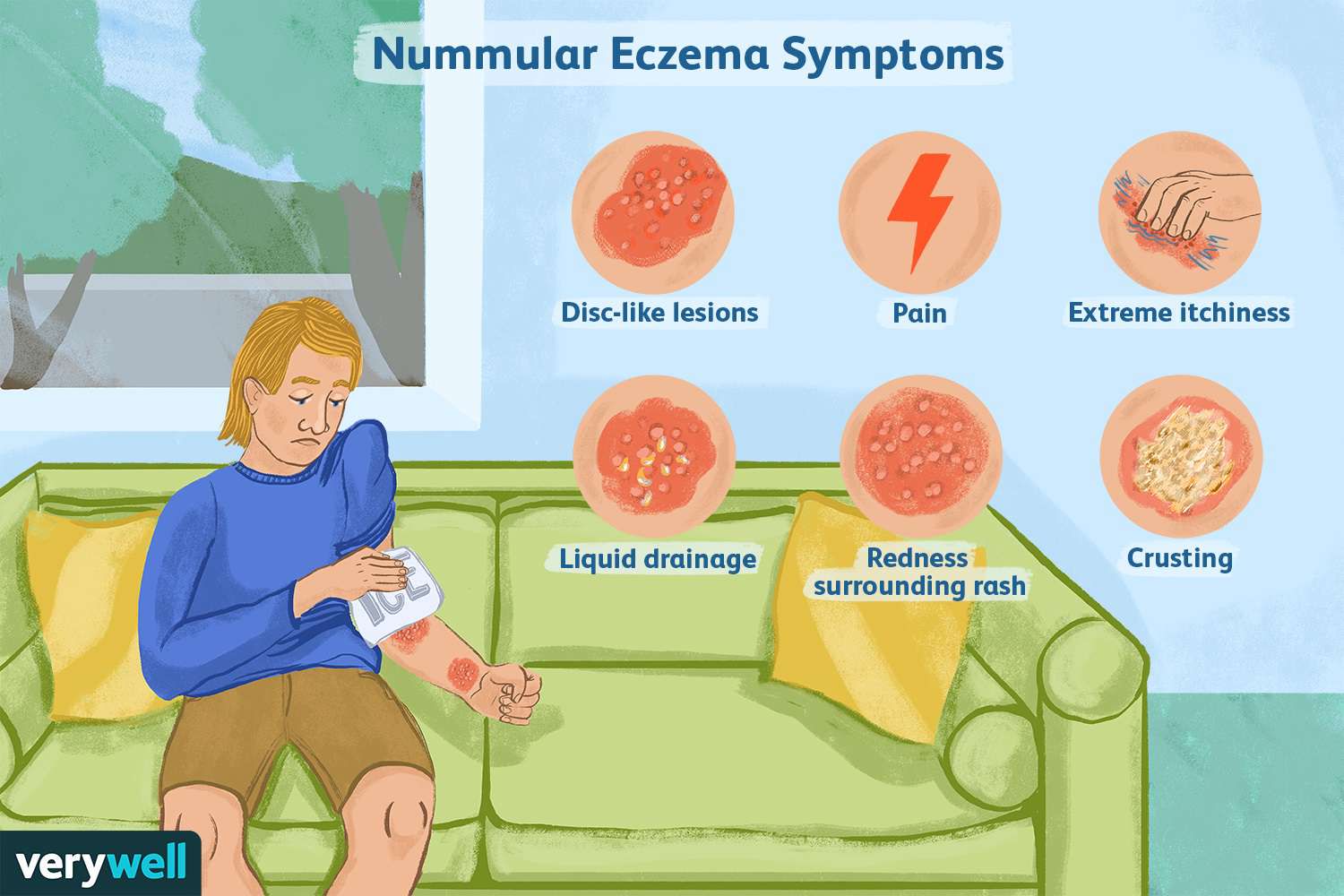
There is no cure for nummular eczema, but there are several ways to effectively manage the condition.
Skin dryness is one of the major factors that contribute to exacerbations. Keeping the skin well moisturized strengthens the barrier protection and reduces the risk of flare-ups.
Here are some tips that can help:
Topical corticosteroids (steroids) are the first-line drug treatment for nummular eczema. Most cases respond well to intermediate- to high-potency steroids, often bringing flare-ups under control within one to four weeks.
Topical steroids are generally applied to affected skin two to four times daily. Ointments are often preferred over gels as they have emollients that help moisturize the skin.
The main goals of treatment are to clear your skin and ease your discomfort. To do this, your treatment plan may include treatment designed to:
Hydrate your skin: It’s likely that you have extremely dry skin. To add moisture to your skin, which will help heal your skin, you may need to:
Moisturizer plays a key role in healing your skin. Your dermatologist may recommend a hypoallergenic, fragrance-free moisturizing cream or ointment instead of a lotion. Creams and ointments do a better job of trapping water in your skin than do lotions. Having more water in your skin can help you heal faster.
Some bath oils can irritate your skin, which can worsen nummular eczema.
Avoid irritating your sensitive skin: Dry, sensitive skin is more likely to have frequent flare-ups of nummular eczema. For this reason, your treatment plan may include instructions that can help you avoid irritating your skin.
You may need to: