Winkelwagen
U heeft geen artikelen in uw winkelwagen
Erythema multiforme affects less than 1% of the population. It is most common in young adults (aged 20–40 years) with a modest predominance in males. There is no association with race.
Mycoplasma pneumoniae infection is often listed as a trigger of erythema multiforme, however mucocutaneous rash and mucositis (MIRM).
Medications which may trigger erythema multiforme include:
Le triméthoprime-sulfaméthoxazole (cotrimoxazole ou TMP / SMX) est couramment utilisé pour le traitement des voies respiratoires urinaires ou inférieures Les infections. Une revue détaillée de la littérature mondiale sur les effets indésirables de TMP / SMX depuis sa première utilisation en 1968, lorsque Des préoccupations ont été exprimées au sujet d’une éventuelle toxicité hématologique. Les réactions indésirables au TMP / SMX se produisent chez environ 1% à 3% des personnes population générale. Ici, nous rapportons un cas d’érythème polymorphe oral (EM) secondaire à TMP / SMX qui présentait des ulcérations orales et lombaires Typique de l’EM sans aucune lésion cutanée et met en évidence l’importance de les distinguer des autres troubles ulcératifs impliquant des voies orales cavité. Le patient a été traité de façon symptomatique et administré une prednisolone au comprimé. La condition s’est améliorée avec l’arrêt de la thérapie TMP / SMX. Il a été signalé que les attaques primaires d’EM oral se limitent à la muqueuse buccale, mais les attaques suivantes peuvent produire des formes plus sévères De EM impliquant la peau. Par conséquent, il est important d’identifier le diagnostic et la gestion précoces. Bien que EM soit assez courant avec TMP/SMX, il n’y a pas de rapports d’EM oral apparaissant après l’admission de ce médicament.
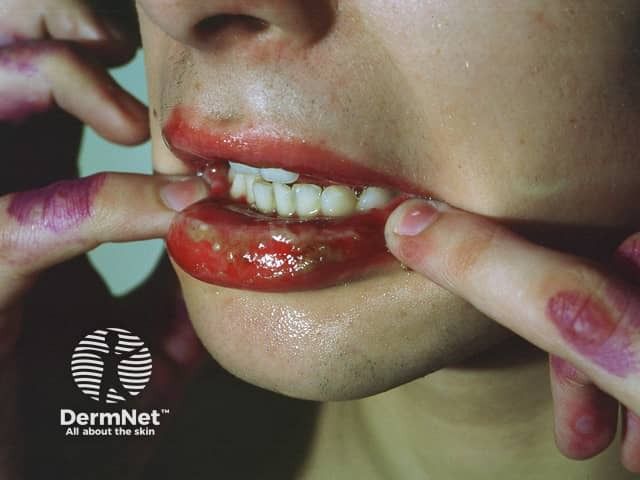
A 20-year-old female presented with complaint of superficial erosions and burning sensation in oral cavity for 5 days, swelling, crusting, and bleeding over lips and difficulty in swallowing for 4 days. Eight days back she was started on oral TMP/SMX (160/800 mg [1 double strength tablet] twice daily by a private physician for urinary tract infection). There was no history of abdominal pain, urinary complaints, breathlessness, or cough. On examination, heart rate was 110/min, respiratory rate was 24/min and blood pressure was 110/70 mmHg. Intraoral examination showed extensive, irregular ulcerations with yellow base and erythematous borders on buccal mucosa, palate, dorsal, and ventral surfaces of the tongue. On extraoral examination, both upper and lower lips showed extensive irregular ulcerations and cracking and fissuring with blood encrustation [ Figure 1 ]. Nikolsky's sign was negative. Systemic examination was normal. A clinical diagnosis of TMP/SMX-induced oral EM was made. This can be considered as a “probable” adverse drug reaction (ADR) as per causality assessment, on Naranjo scale.[6] Biopsy was taken from buccal mucosa and for culture test, sample was collected from mucosal lesions. Patient was advised to discontinue the TMP/SMX therapy and was treated with oral antihistamines, analgesics, and topical triamcinolone acetonide gel (0.1%) for the oral ulcers. After this, patient was referred for laboratory investigations. The pathology report which came on the next day stated an EM-type drug eruption. Histopathological report showed lymphocytic infiltrate at the epithelial-connective tissue junction and around blood vessels with edema and subepidermal bullae formation [ Figure 2 ]. Her hematological investigation which was came after 3 days showed neutrophilia and eosinophilia. C-reactive protein was positive and the erythrocyte sedimentation rate was elevated. Serology tests confirmed that the patient was negative for herpes virus infection. Furthermore, the culture test came as negative. Liver function tests, renal function tests, and serum electrolytes were normal. HIV – enzyme-linked immunosorbent assay was negative. Depending on the history, clinical examination and laboratory investigations, a final diagnosis of drug-induced oral EM was given. Patient was then prescribed corticosteroids (prednisolone 10 mg) twice a day for 3 days followed by tapering dose for 10 days. By the end of the 3 rd week, there was no evidence of mucosal lesions. Rechallenge with TMP/SMX was not performed. On follow-up, after 4 months, she is asymptomatic.
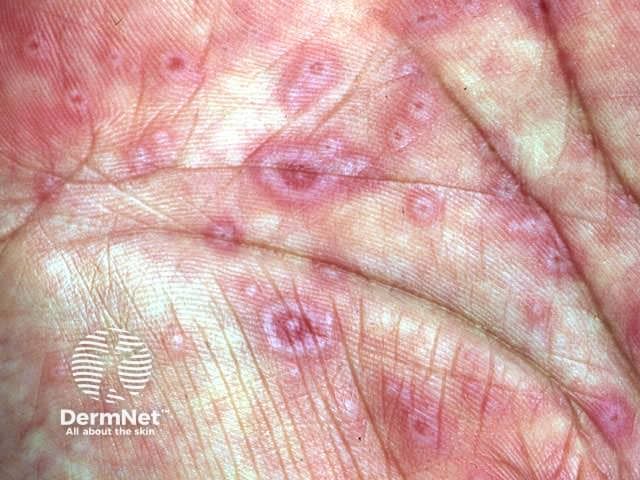
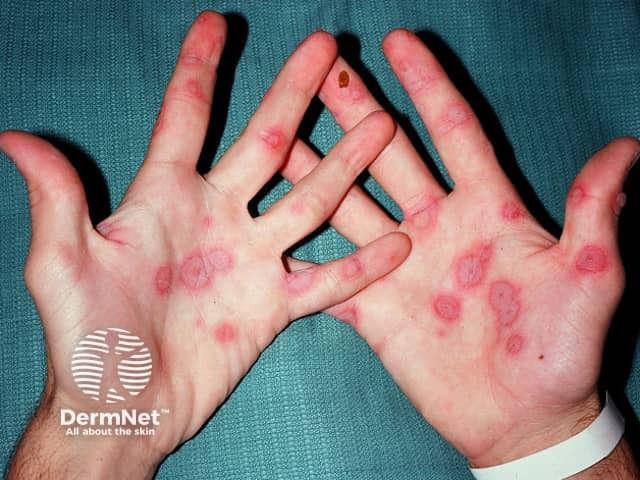
Erythema multiforme kan op elke leeftijd optreden. In 80% van de gevallen is de aandoening niet ernstig en voelt men zich niet ziek. De huidafwijkingen worden vooral gezien op de handen (zowel de handruggen als de handpalmen), de polsen, de voeten, de ellebogen en de knieën. De huiduitslag van erythema multiforme kan bestaan uit vlekken, bobbeltjes, galbulten, zogenoemde ‘schietschijven’ of een combinatie daarvan. Deze huidafwijkingen zijn rood van kleur, kunnen klein blijven maar ook wel 3 centimeter groot worden.
Soms zijn er maar enkele huidafwijkingen, soms is de uitslag zeer uitgebreid. In het laatstgenoemde geval is er sprake van een ernstiger aandoening het Stevens-Johnson syndroom, waarbij de patiënt ook ziek kan zijn. Daarnaast doen dan ook de slijmvliezen mee, meestal van de mond en soms andere slijmvliezen (geslachtsorganen, ogen).
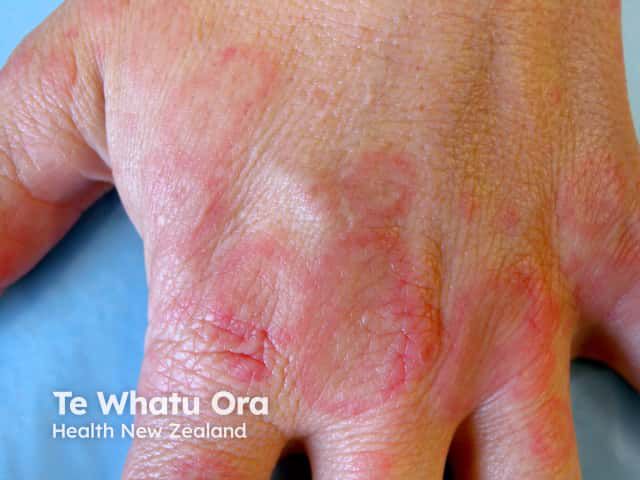
Erythema multiforme (EM) is a cutaneous and mucosal hypersensitivity reaction with characteristic lesions triggered by certain antigenic stimuli. It represents an acute, sometimes recurrent condition of the skin and mucosal membranes manifested by papular, bullous, and necrotic lesions. Its causes are variable and numerous, and its evolution is generally favorable.[1][2][3][4]
Most lesions appear in 48 to 72 hours and favor the extremities. The lesions remain localized to one site and heal within 7 to 21 days. Common precipitating factors include herpes simplex virus, histoplasmosis, and Epstein Barr virus. Recurrences are not uncommon if the trigger is Herpes simplex. While most cases are mild, severe cases can be life-threatening. The mucous membranes are involved in 2 to 10% of individuals. Overall, the majority of cases of EM are linked to medications.
EM is often associated with viral or bacterial infections, especially HSV. Studies have demonstrated the presence of HSV-DNA by a polymerase chain reaction in acute or sequellae EM lesions. The predisposing factors are unknown. HLA-DQ3 is reported to be associated with postherpetic EM and has been suggested as an additional diagnostic marker. Other human leukocyte antigen groups have also been reported as markers of recurrent EM.
The damage to the epithelial cells is via cell-mediated immunity. During the early phase of the disease, there is an influx of macrophages and CD8 T lymphocytes, which release a wide range of cytokines that mediate the inflammation and resultant cell death.
When the process is due to drug hypersensitivity, the earliest pathological feature is necrosis of keratinocytes.