Winkelwagen
U heeft geen artikelen in uw winkelwagen
As highlighted in previous studies, FDLPPPS is a not uncommon presentation for dermatologists specializing in conditions affecting the hair. Trüeb et al. (9) were the first to report on the bi-phasic nature of FD based on their sequential dermoscopic observations in FD. Yip et al. (5) described this clinical presentation in 13 patients for the first time in 2019, Egger et al. (7) studied 7 patients shortly after, and Müller-Ramos et al. (10) described 2 paediatric cases. However, some case reports describing patients with clinical overlap between LPP and FD (11–13) suggest that clinicians might encounter FDLPPPS cases more often than currently believed. To our knowledge, this study describes the largest series of FDLPPPS in the literature to date.
The scarce symptoms associated with this condition are also notable. Pruritus was found in less than the half of our patients and trichodynia in only 3 cases. This is much less frequent than symptoms associated with FD (68% of the patients have associated pruritus and 30% trichodynia).
The use of oral antibiotics in FD is controversial due to increasing antibiotic resistance (17), in our series, most of the patients were taking oral doxycycline or the combination of oral clindamycin and rifampicin. Both options have demonstrated to induce a significant improvement in FD during 4.8–7.2 months, respectively (8, 18). Oral antibiotics could be necessary to induce a prolonged remission in acute stages of FD that, at some point, is followed by a definitive change to the chronic lichenoid stages of FDLPPPS.
The treatment may be different once the FDLPPPS is established. Recent investigations have shown that the role of Staphylococcus aureus might be less relevant in FDLPPPS forms, and anti-inflammatory treatments should be prioritized (19). In the current study, the options most used were topical and intralesional steroids, followed by topical antibiotics. The oral treatment is not well defined, but immunomodulatory therapeutic options are used more often (e.g. oral isotretinoin, hydroxychloroquine, dexamethasone and cyclosporine). In our experience, FDLPPPS is easier to control than the FD or the LPP classical forms, which means a better prognosis for patients in this stage. The authors propose a therapeutic approach in Fig. 4 that combines those used in FD and classic LPP, based on the degree of inflammatory activity and the course of alopecia. The low number of cases of reactivation of FD do not allow further analysis. However, the treatment in those patients was almost stopped and totally interrupted in 4 cases.
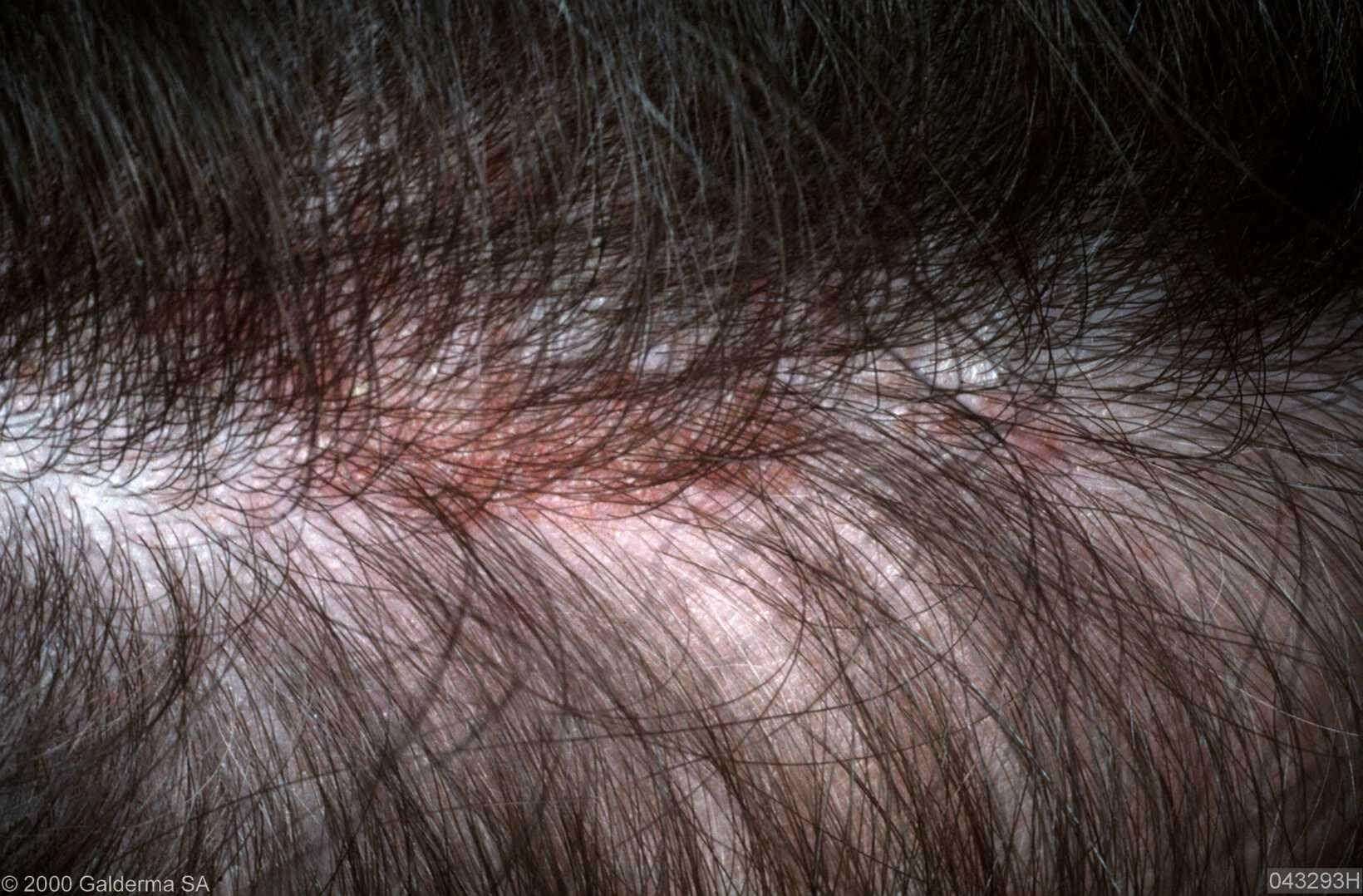
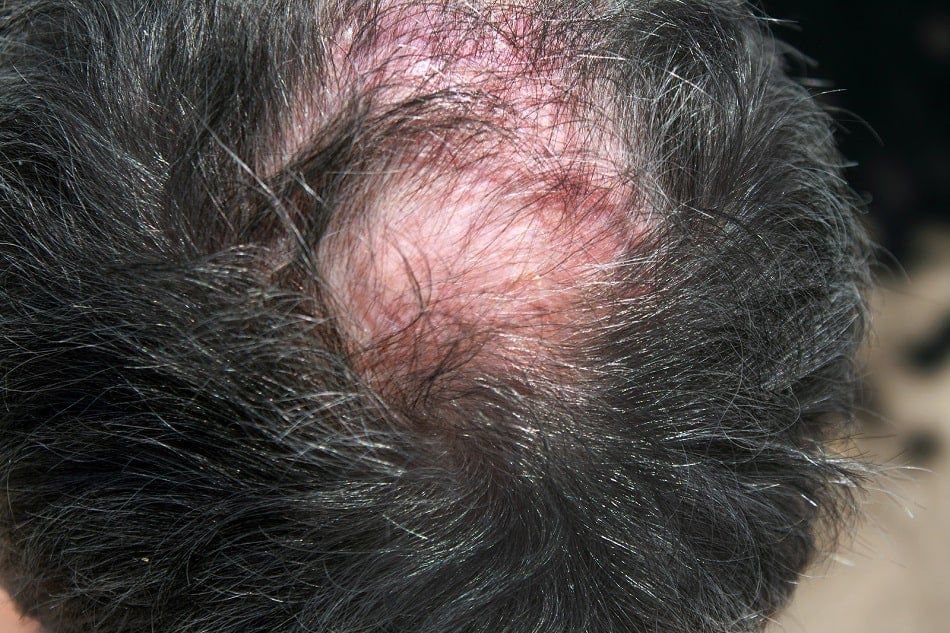
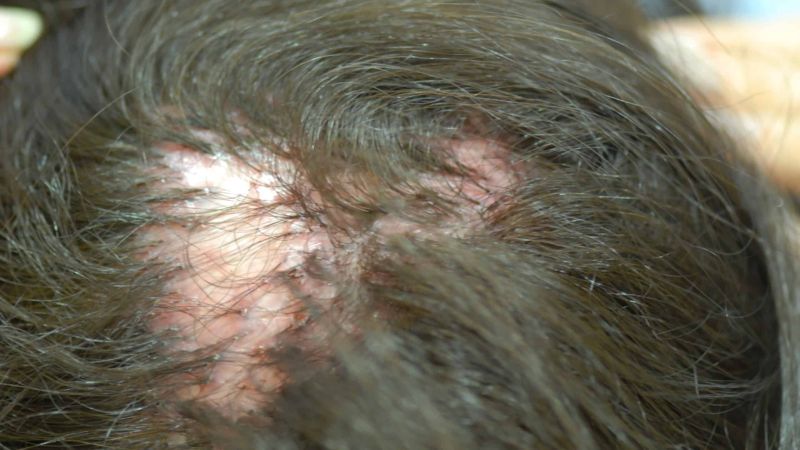
Folliculitis delcavans is a rare ailment that causes red, swollen patches on your scalp. The patches destroy your hair follicles, causing scars and permanent hair loss at the affected sites.
While there is no known cause, the problem is linked to a bad response to Staphylococcus A. bacteria. It is believed that the bacteria trigger an extreme immune response that causes symptoms.
Treatments can reduce symptoms and slow the damage to hair follicles. The nature and chronic course of this problem can also have a negative impact on those who have it. Enduring long-term treatment only to have the problem recur can be difficult. This can also have an impact on your self-image and affect your quality of life.
Working with your healthcare provider and a counselor can help you manage the mind and body aspects of this problem. Despite its long course, the outlook is good for most cases.
Verywell Health uses only high-quality sources, including peer-reviewed studies, to support the facts within our articles. Read our editorial process to learn more about how we fact-check and keep our content accurate, reliable, and trustworthy.

This is an open access article distributed under the terms of the Creative Commons Attribution License CC-BY 4.0., which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
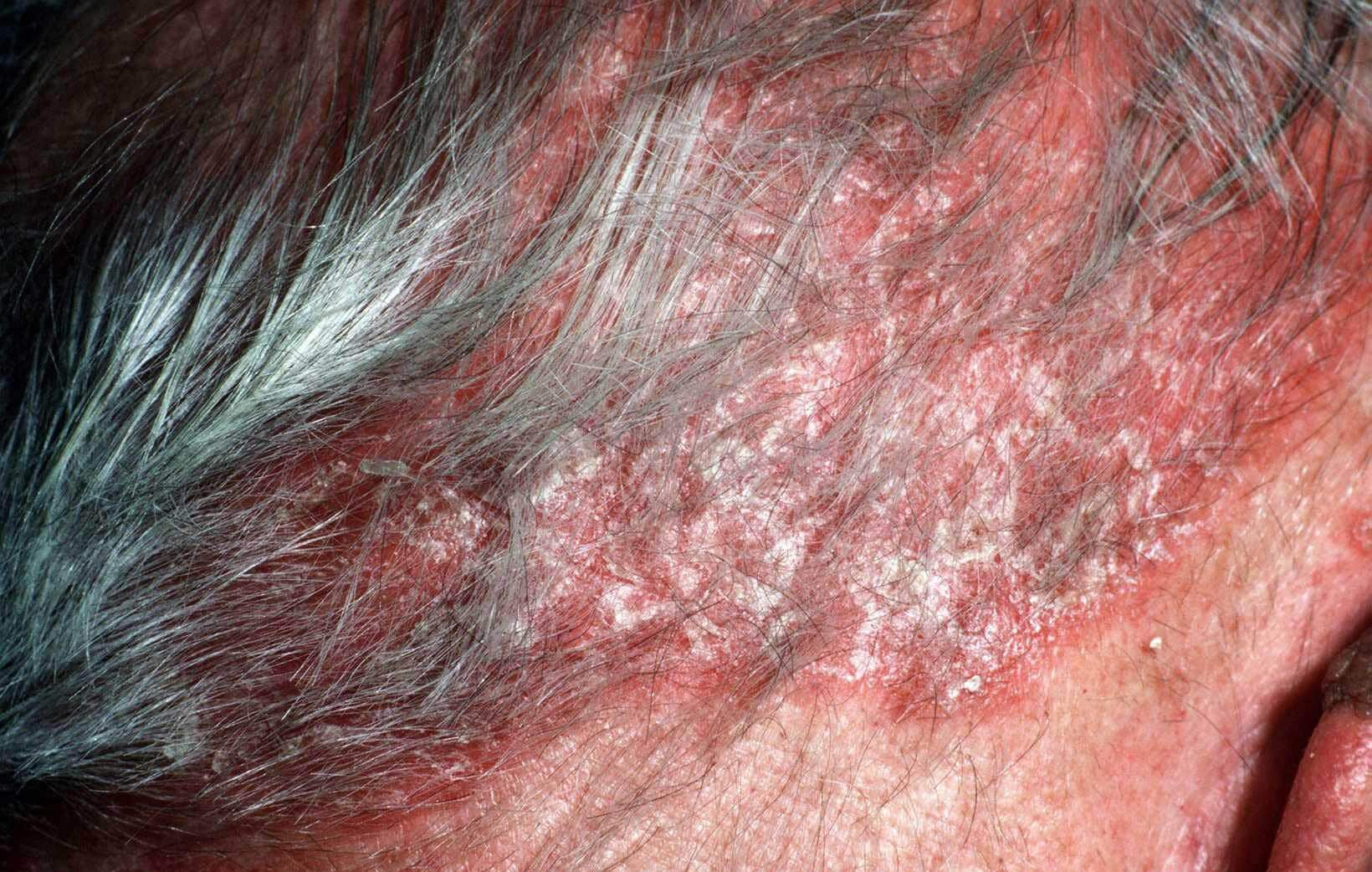
Folliculitis decalvans (FD) is a rare type of inflammatory scalp disorder that leads to scarring alopecia. It is classified as primary neutrophilic cicatricial alopecia. FD presents a challenging scenario in clinical dermatology due to its rarity, resistance to treatment, and potential for scarring alopecia. This inflammatory scalp disorder primarily affects middle-aged adults, predominantly males. While its exact pathogenesis remains uncertain, a deficient host immune response to Staphylococcus aureus infection is hypothesized. Therapeutic interventions for FD pose difficulties, with limited treatment options available
A 58-year-old female patient presented with a history of follicular papules that gradually progressed to form clusters of pustules, crusting, and hemorrhagic lesions with tufting of hairs on the crown area of the scalp, and was diagnosed with FD. Considering isotretinoin's role in inhibiting abnormal keratinization and inflammation, and rifampicin's ability to eradicate S. aureus, the combination of both provides a comprehensive approach to tackling the underlying factors contributing to FD. Despite previous unsuccessful treatments, combination therapy with isotretinoin and rifampicin yielded a remarkable outcome, prompting further exploration of this approach.
Keywords: alopecia, cicatricial alopecia, combination therapy of isotretinoin and rifampicin, rifampicin, isotretinoin, folliculits decalvans

Tetracycline (z.B. Tetracyclin-Wolff) initial 1 g/Tag p.o., später Reduktion auf 500 mg/Tag. Therapieversuch mit Isotretinoin (z.B. Isotretinoin-ratiopharm, Aknenormin) 0,5 mg/kg KG/Tag.
Alternativ Clindamycin/Rifampicin: In einigen Fällen werden gute Therapieeffekte mit der Kombination von Clindamycin und Rifampicin beschrieben (Bunagan MJ et al. 2015): Clindamycin/Rifampicin 300mg 2x/Tag über 10 Wochen (Vañó-Galván S et al. 2015).
Alternativ Orale Fusidinsäure (3x500mg/Tag) über eine Zeit von 3-4 Monaten (Pimenta R 2019).Einzelfallberichte zeigten positive Erfolge mit einer Kombinationstherapie von Dapson (100 mg/Tag) und Isotretinoin (1 mg/kgKG/Tag) sowie von Adalimumab (Shireen F et al. 2018).
Alternativ Isotretinoin: Bei der seltenen Kombination mit einer Acne vulgaris ist eine Therapie mit Isotretinoin empfehlenswert.
Bei stärkerer Entzündung kurzfristig Glukokortikoide in mittlerer Dosierung 60-80 mg/Tag (z.B. Decortin H) in abfallender Dosierung.