Winkelwagen
U heeft geen artikelen in uw winkelwagen
Numerous factors may influence an individual’s risk of developing P. aeruginosa folliculitis from an environmental exposure. These risk factors include changes to cutaneous flora, female gender, length of exposure, and skin trauma. It would be impractical to recommend all women avoid extended hot tub use. Additionally, patients with unhealed thermal burns of skin are not likely to use hot tubs or public pools. Thus, counseling should be directed to those with diabetes, immunocompromised states, or trauma of the skin. These populations can be educated on the risk of infection with extended submersion in public pools or hot tubs.
The content published in Cureus is the result of clinical experience and/or research by independent individuals or organizations. Cureus is not responsible for the scientific accuracy or reliability of data or conclusions published herein. All content published within Cureus is intended only for educational, research and reference purposes. Additionally, articles published within Cureus should not be deemed a suitable substitute for the advice of a qualified health care professional. Do not disregard or avoid professional medical advice due to content published within Cureus.
The authors have declared that no competing interests exist.
Hot tub folliculitis ( Pseudomonas folliculitis ), or "hot tub rash," is a bacterial skin condition you can get from using an improperly maintained hot tub or swimming pool. It causes a red, itchy, and bumpy rash anywhere from a few hours to a few days after being in the water.
Hot tub folliculitis is caused by the bacteria Pseudomonas aeruginosa, which infects the hair follicles. The bacteria is commonly found in recreational water and natural sources of water, such as lakes and rivers. It is also frequently caused by Staphylococcus aureus and the fungus Aspergillus Nigus.
This article covers the symptoms and causes of hot tub folliculitis. It also discusses how it is diagnosed, treatment options, and prevention tips.
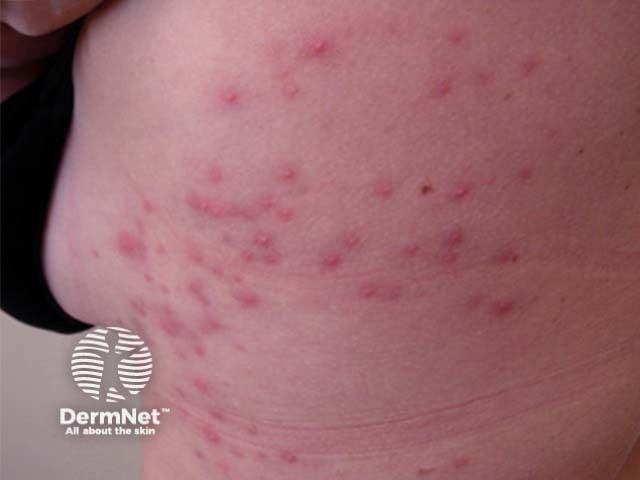
Pseudomonas aeruginosa cannot survive on healthy skin, so the rash usually resolves on its own after seven to 10 days. Treatment, if needed, can include home or over-the-counter (OTC) remedies, or prescription medications. However, hot tub rash often clears up on its own within 10 days.
Until then, several home remedies may help relieve symptoms and speed up healing. Ask your healthcare provider before trying any of these home treatments for hot tub rash:
If home care isn't doing the trick, or if your rash is severe, your healthcare provider may prescribe a topical antimicrobial such as gentamicin cream or Polymyxin B spray. For widespread, resistant cases of hot tub rash, the oral antibiotic Cipro (ciprofloxacin) can be prescribed.

There are no specific tests for folliculitis. If you see a healthcare professional they will ask questions (a medical history) and examine the rash to try and decide whether you have folliculitis and why it has happened. In some cases, for example if you have had treatment and it has not helped, they may take a sample of any pus or crusting (a swab) and send it to the laboratory. This tries to help identify the cause of the rash and what treatment you may need.
Identifying the cause of the folliculitis will help decide what will help. General measures include:
Most cases or folliculitis are mild and do not need any treatment. It often clears without any treatment within 7-10 days. It may be helpful to use a moisturiser (emollient) which contains an antibacterial agent - for example, Dermol® cream or lotion or Emulsiderm®. It may help the folliculitis to clear more quickly and reduce the risk of it becoming worse.
You can use one of these emollients as a soap substitute until the folliculitis has cleared. Specific preparations for the bath or shower are available - for example, Dermol® 200 Shower Emollient, Dermol 600® Bath Emollient and Oilatum® Plus bath additive.
If simple measures over a few days do not allow the folliculitis to improve, you should probably see your GP for further advice and treatment.
For localised areas of folliculitis, an antibiotic cream may be useful. Fusidic acid is a suitable antibiotic cream that can be applied 3-4 times per day to affected areas. If you are thought to have a fungal infection, you may be given a different type of medication.
Für Zugriff auf PubMed Studien mit nur einem Klick empfehlen wir Kopernio
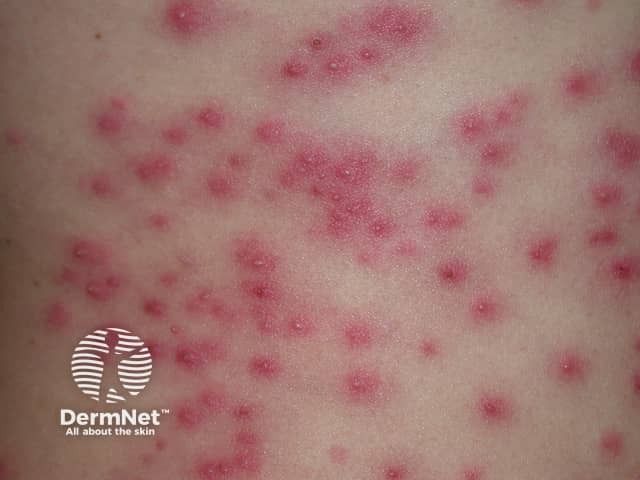
Een uitslag van folliculitis in een bubbelbad is jeukend, hobbelig en rood. Het lijkt op acne, maar de uitslag verschijnt veel sneller.
Wanneer het voor het eerst verschijnt, veroorzaakt hot tub-folliculitis een overvloed aan kleine, korrelige bultjes die papels worden genoemd. Deze papels zijn helder tot donkerrood.
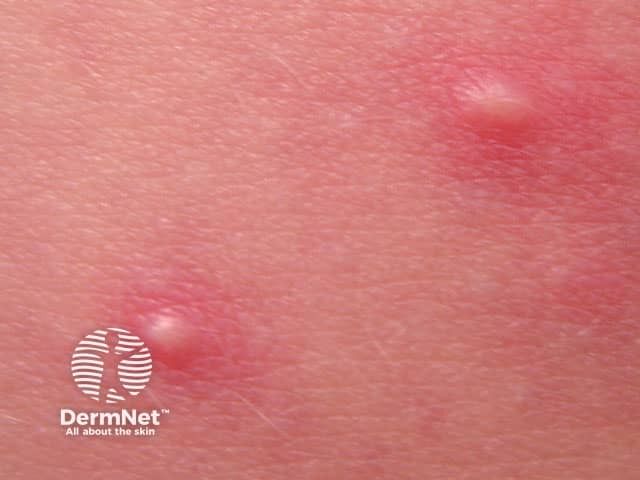
Naarmate de uitslag vordert, worden de bultjes groter en zachtere knobbeltjes die tot drie centimeter in diameter kunnen zijn. De papels hebben centrale puisten en met pus gevulde blaren kunnen zich ook rond de haarzakjes vormen.
Tepels van zowel mannen als vrouwen kunnen geïnfecteerd raken en gezwollen en gevoelig worden. Het komt niet vaak voor, maar sommige mensen met folliculitis in een bubbelbad voelen zich in het algemeen ook onwel en kunnen andere symptomen krijgen, zoals: