Winkelwagen
U heeft geen artikelen in uw winkelwagen
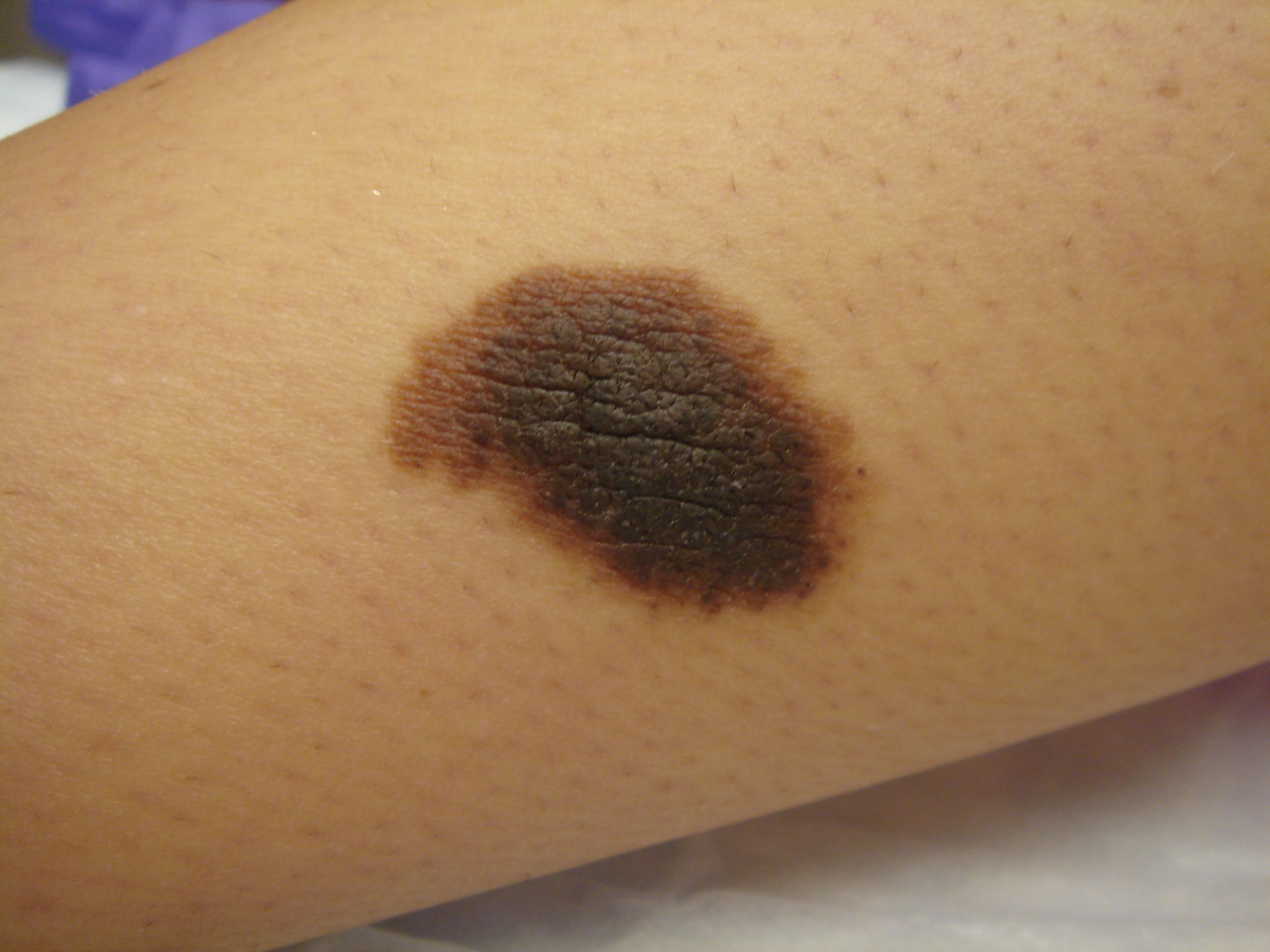
HALO NAEVUS – tiež nazývaný aj ako Suttonov névus je plochý alebo nodulárny névus obsahujúci hnedý pigment , ktorý je obklopený depigmentovaným prstencom alebo „ svätožiarou“. Halo okolo névu je vlastne dvorec vitiliga. Predpokladá sa, že k vzniku halo okolo névu dochádza, keď biele krvinky / CD8 + T lymfocyty / zaútočia a zničia melanocyty / bunky kože produkujúce pigment melanín /. Príčina útoku však nie je známa. Počas leta je nutné Halo naevus chrániť pred slnečným žiarením krémami s vysokým ochranným faktorom SPF 50 +, aby nedošlo k spáleniu svetlých častí.
Ak pigmentová časť Suttonovho névu vykazuje atypické znaky je vhodné odporučiť chirurgický zákrok.
Tatu, A.L, et al. A Study of Halo Naevi, Vitiligo and Asymptomatic Autoimmune Thyroiditis. (2017) Invest Dermatol Venereol Res 3(1): 105- 107.
Halo naevi, Dermoscopy, Vitiligo, Anti-thyroid peroxidase, Autoimmune thyroiditis
Purpose
We sought to assess the association of Hallo Naevi (HN) or of HN-vitiligo with thyroiditis by screening markers of thyroiditis in patients presenting Hallo Naevi (HN) and HN associated with vitiligo.
In this study were included adults patients with halo nævus and / or vitiligo presented in dermatology outpatient clinic between 2010 and 2016. Clinical and dermoscopy examination were performed. The possible association between vitiligo and thyroiditis was assessed by peripheral blood dosage of Anti-Thyroid Peroxidase (ATPO).
Were included 37 patients, 16 female and 21 male. Twenty five patients (67.56%) had one HN, 7 patients(18.91%) had 2 HN and 5(15.31%) of the patients had 3 HN. From 37 patients with halo nevus 10 (27.02%) had associated vitiligo. In all cases vitiligo occurred 3 - 4 years after the onset of HN. In all 10 patients with HN and associated vitiligo, lesions were of non-segmental type: limited, symmetric, small and large lesions of extremities. Among them five had one HN (4 female and 1 male), 2 patients had 2 HN (one male and one female), 3 patients had 3 HN.
In 27 (72.98%) patients with HN ( and no vitiligo): ATPO peripheral blood levels were normal in 26 patients (96.29%), a 13 years old boy had high ATPO (presented in the discussion) (3.71%).
In 10 patients with HN and associated vitiligo: 3 had high ATPO results (33.33% of patients,1 male with 2 HN and 2 female with 3 HN) with a 2/1 female/male ratio. One of female with 3 HN had a history of autoimmune thyroiditis and vitiligo - both occurred after the onset of HN (by order thyroiditis, HN then vitiligo). In 2 others cases with high ATPO clinical appearance of the conditions was HN, vitiligo and thyroiditis. Vitiligo features were in all cases of type non-segmental with bilateral hypo-chromic, symmetrical small macules (0.3 - 0.8 cm diameter) and Koebner phenomena or large plaques located on extremities (Figure 1).

HN-associated vitiligo is more likely to present in certain populations and with certain clinical features. A retrospective study of 101 patients with HN-associated vitiligo demonstrated that risk factors for developing vitiligo in patients with HN include: 1) Koebner phenomenon, 2) multiple HN, and 3) family history of vitiligo [6]. A prospective study of 553 patients with HN-associated nonsegmental vitiligo (n=130) and generalized vitiligo (n=423) showed that age
Our patient also had diffuse PHG. Lesional leukotrichia associated with vitiligo patches or HN of the scalp can result in focal graying of hair. However, diffuse PHG is uncommon. and family history of PHG may be seen in patients with nonsegmental HN-associated vitiligo [1,6]. However, reports of PHG occurring concurrently in a patient with an acute disseminated presentation of HN-associated vitiligo are lacking. PHG is an inherited trait, it is likely triggered by an early reduction in tyrosinase function in the melanocytes of the hair bulb and associated with defective migration of melanocytes in follicular papilla, and faulty melanocyte-cortical keratinocyte interactions [1]. However, genetic polymorphisms may suggest a possible immunological factor [7], targeting hair follicle melanocytes implicated in a subset of cases [1]. Nevertheless, PHG is a very unusual finding in a patient with HN-associated vitiligo. In patients with multiple HN, PHG may represent a robust immune response that warrants a search for melanoma as a possible trigger due to its association with multiple new HN [8]. Total body skin and ophthalmological exam were non-concerning in our patient.
Our patient’s acute clinical presentation of disseminated HN-associated nonsegmental vitiligo and diffuse PHG represents a rare presentation of vitiligo. While PHG may be related to an autoimmune/autoinflammatory process, it is not thought of as such. Thus, further research of the pathophysiology and clinical course of these findings in the context of HN-associated nonsegmental vitiligo may guide management and provide insights into disease prognosis.

A Wood lamp, which emits UV light with a wavelength of 365 nm, is helpful in diagnosing nevus anemicus. The lamp does not accentuate the hypopigmentation of nevus anemicus but does accentuate the hypopigmentation and depigmentation seen in nevus depigmentosus and vitiligo, respectively. A skin biopsy may be performed, which may reveal normal skin, thereby ruling out other hypopigmented or depigmented lesions such as vitiligo.
Electron microscopy findings of nevus anemicus are normal, whereas nevus depigmentosus shows a normal number of melanocytes but decreased melanization with melanosome aggregation in melanocytes. If tinea versicolor is suspected, potassium hydroxide (KOH) examination of lesional skin should be performed, revealing the characteristic "spaghetti and meatballs" appearance of Malassezia furfur hyphae and spores, respectively.
Deterrence and patient education regarding nevus anemicus are centered on dispelling misconceptions and promoting understanding of this benign condition. Healthcare providers play a crucial role in educating patients and caregivers about the harmless nature of nevus anemicus, emphasizing its stable course and lack of associated health risks. Patients should be informed that nevus anemicus does not require active treatment unless for cosmetic reasons, and interventions such as laser therapy are generally ineffective.
Key clinical pearls of nevus anemicus provide essential insights into its benign nature, varied presentations, and management implications, as mentioned below.
Congenital onset: Most commonly observed at birth or during early childhood and remains stable throughout life.
Benign nature: Generally asymptomatic and benign, with no associated systemic complications or health risks.
Diagnosis: Clinical diagnosis is based on characteristic features, differentiation from other hypopigmented conditions like vitiligo and nevus depigmentosus is crucial.
Association with NF1: In some cases, nevus anemicus may be associated with NF1, necessitating further evaluation if other NF1 features are present.
Psychosocial impact: Educating patients about the harmless nature of the condition is essential to alleviate anxiety related to its appearance.
Consultations: Dermatological consultation is recommended for diagnosis confirmation.