Winkelwagen
U heeft geen artikelen in uw winkelwagen
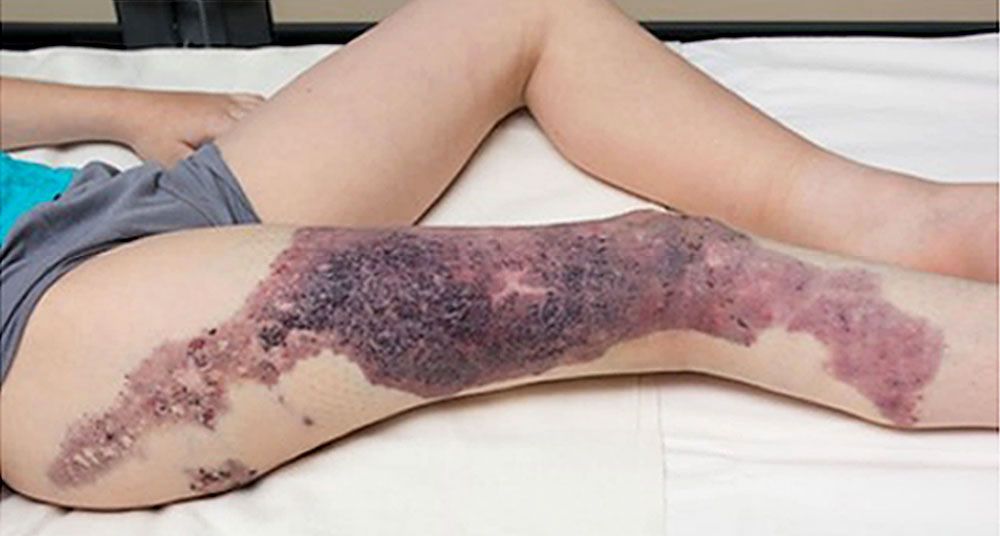
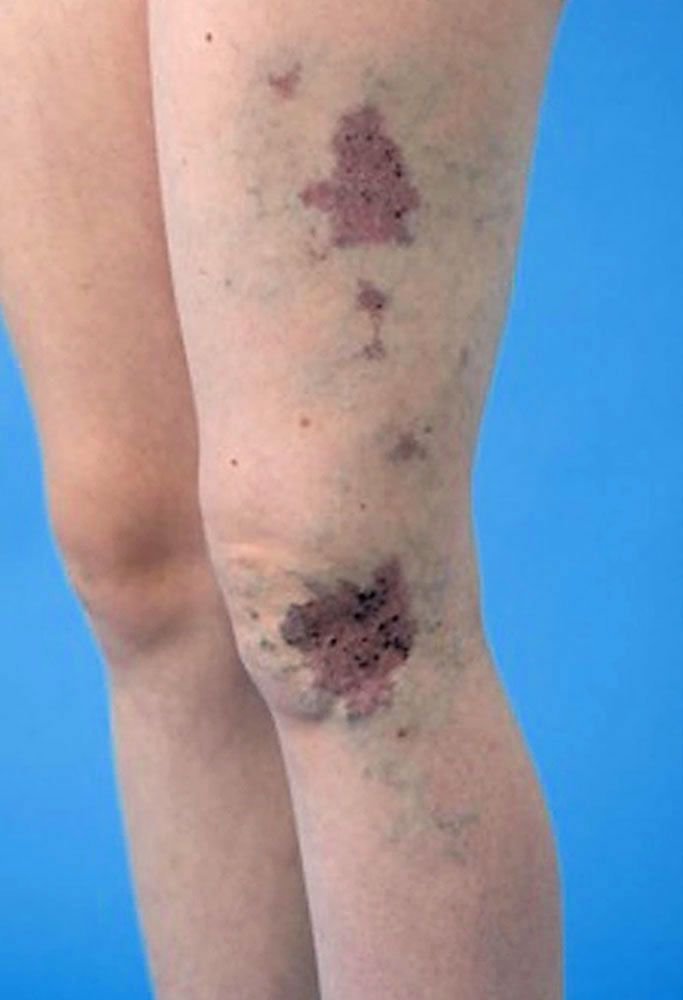
Cutaneous haemangioma seen on left thigh of a patient with Klippel-Trénaunay syndrome (limit of edges outlined by blue arrows).
Lateral marginal vein (blue arrows) and gluteal vein (yellow arrow) seen in patient with Klippel-Trénaunay syndrome. The lateral marginal vein is considered pathognomonic of the disease.
MRI showing lateral marginal vein (yellow arrow), perforator vein (blue arrow) and an isolated segment of a vestigial or hypoplastic femoral vein (red arrow).
Lymphatic malformations, which are more common than expected, occur in 11% of KTS patients. They consist of dilated vessels filled with clear protinaceous fluid, but they do not connect to normal lymphatic vessels lying in cutaneous and subcutaneous tissue. 8 The lymphatic system has a very close developmental, structural and functional relationship with the venous system, 9–11 and plays an important role in the symptomatology and progress of these patients. It is best imaged by MRI- lymphangiography. 9
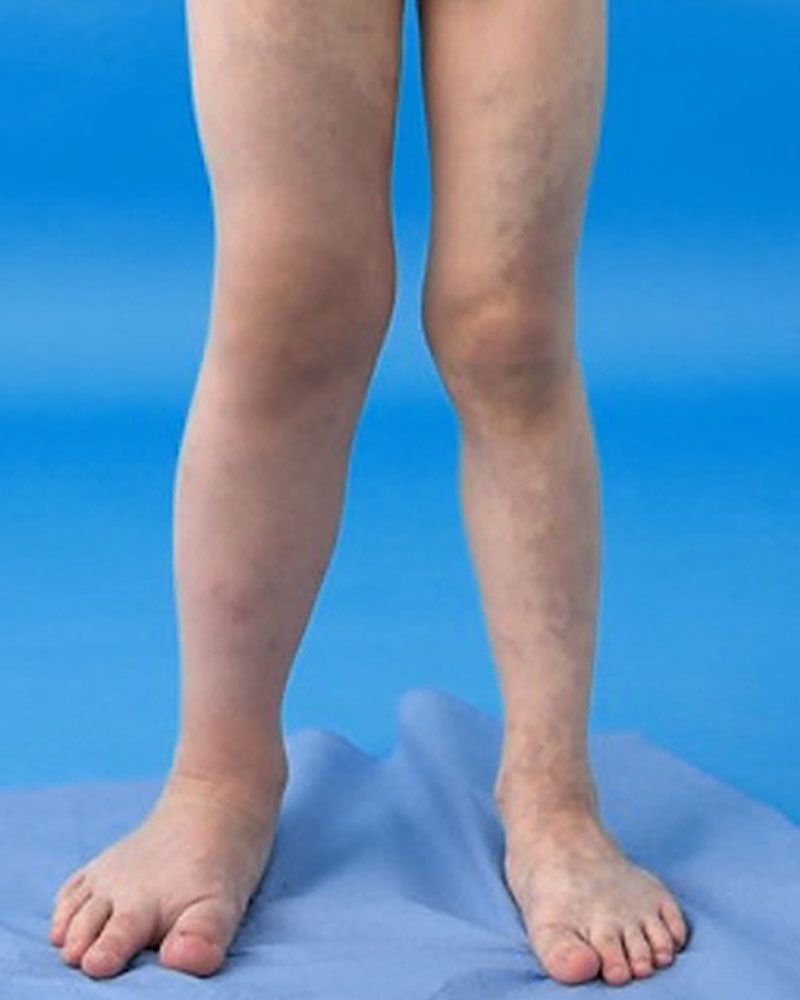
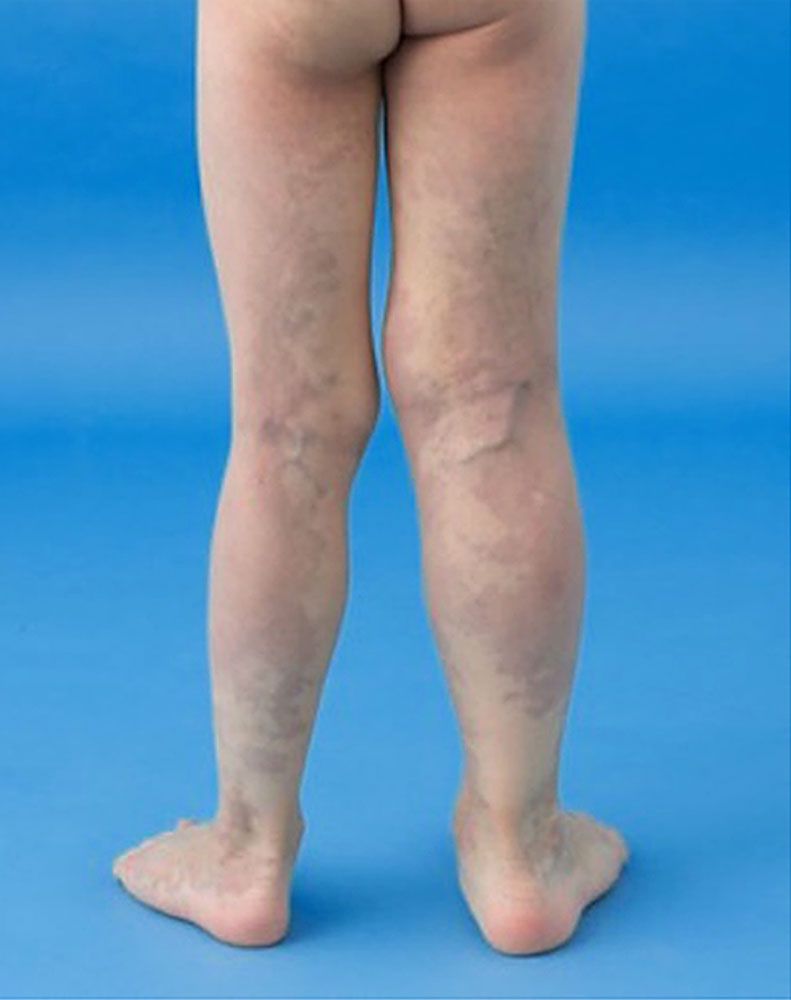
Limb hypertrophy occurs in 67% of KTS patients, with 88% involving the lower limb 2 and 71.5% involving a single limb 6 [ Figure 4 ]. Though bilateral and truncal involvement are rare, extensive venous networks extend to spread across viscera of the pelvis and spinal cord. 12 Visceral vascular malformations can be seen in the liver, bladder, rectum, retropeitoneum and pericardium. 4 Patients can therefore present with a variety of symptoms including internal haemorrhage and rectal bleeding. 13
Beim Klippel-Trenaunay-Weber-Syndrom handelt es sich um einen Symptomkomplex, der angeboren ist. Dabei treten Missbildungen am Gefäßsystem auf. Ein weiteres Merkmal sind erhebliche Wachstumsstörungen an den Armen und Beinen. Die Erkrankung trägt auch die Bezeichnungen Klippel-Trenaunay-Syndrom, angiektatischer Riesenwuchs oder Angio-osteohypertrophisches Syndrom.
Das Klippel-Trenaunay-Weber-Syndrom ist angeboren und zeigt sich nur sehr selten. So konnten bislang erst circa 1000 Krankheitsfälle dokumentiert werden. Benannt wurde das Syndrom nach den französischen Ärzten Maurice Klippel (1858-1942) und Paul Trenaunay (1875-1938), die die Erkrankung erstmals beschrieben. Anteil an dieser Beschreibung hatte zudem der englische Mediziner Frederik Parkes Weber (1863-1962).
Patients with Klippel-Trenaunay syndrome need to be aware of the progressive nature of this condition. In children who are diagnosed with KTS, parents need to be educated on possible complications and to ensure close follow-up to monitor for limb length discrepancy and timely management. Patients should be educated on proper skin care to prevent complications arising from superficial infection. Patients scheduled for elective surgeries should be aware of the need for anti-thrombotic prophylaxis two weeks prior to surgical procedures. Pregnant women need to be closely monitored for higher risk of thrombosis. Education should be provided to seek immediate medical education for acute gastrointestinal bleeding.
Klippel Trenaunay syndrome is a complex vascular malformation syndrome with multi-system involvement. A collaborative approach among health care professionals is important to provide optimal care for these patients. The diagnosis is usually considered by the pediatric provider as clinical findings are often seen in the neonatal period and throughout childhood. Referral to a dermatologist for confirmation of the diagnosis and consultation with radiologists can aid in the appropriate evaluation of these patients. Patients with limb length discrepancy may benefit from orthopedic expertise for orthotics or epiphysiodesis and in cases of severe hypertrophy de-bulking procedures.
Hematologists are often involved due to the high risk of thrombosis and the need for prophylaxis during surgeries. Vascular surgery involvement may be required for chronic venous insufficiency for sclerotherapy and, in refractory cases, open surgical procedures. Larger institutions have specialized clinics for patients with Klippel-Trenaunay consisting of a multi-disciplinary team, including dermatologists, orthopedists, dermatologists, and vascular surgeons. Medical and surgical care should be tailored to each patient, depending on the extent of the disease involvement. The primary care provider plays an important role in coordinating care among various specialists to optimize outcomes.
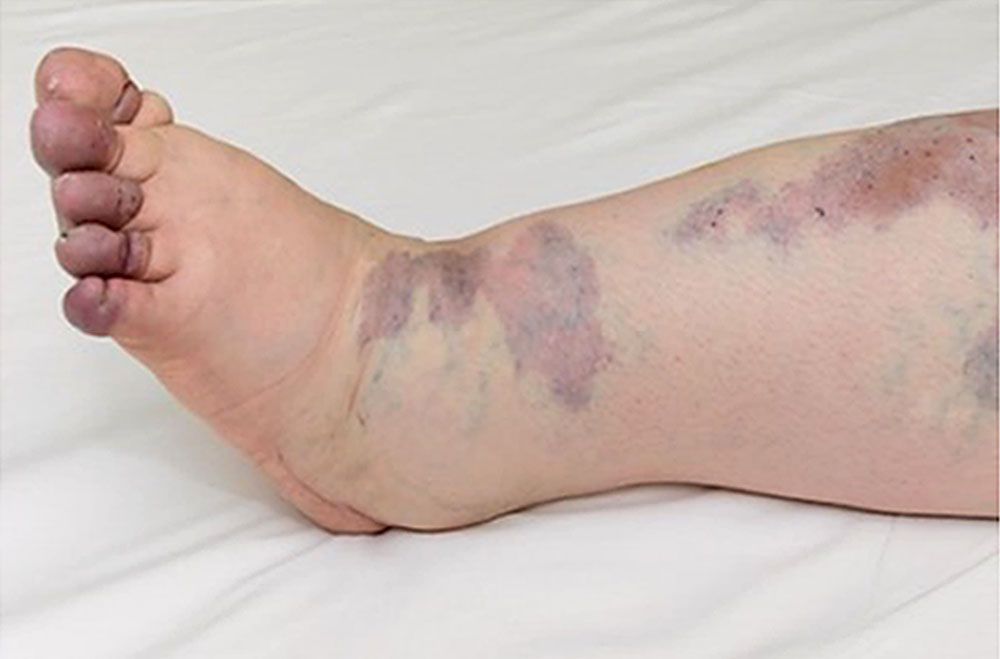
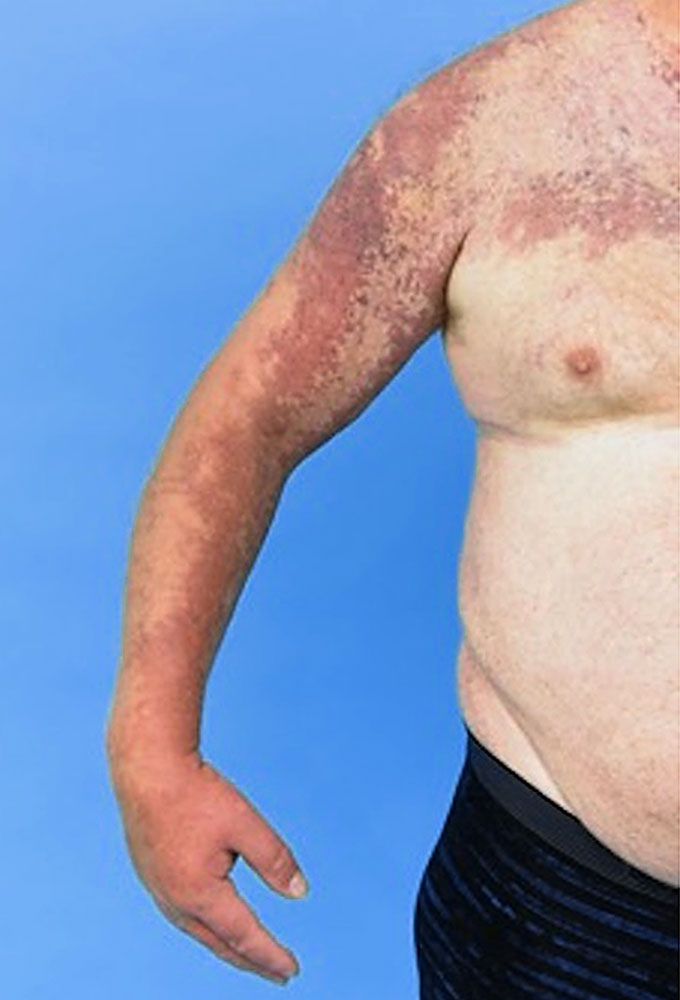
KTS without lymphatic involvement is diagnosed as diffuse capillary malformation with overgrowth (DCMO), which presents with more proportionate overgrowth and diffuse or reticulate stains [5]. The mosaic mutation can occur at any stage of in utero developmental process, and the severity of KTS depends on the timing of this mutation during this developmental stage. If this mutation occurs early in the developmental stage, it will cause severe disease expression after birth. At birth, patients usually present with a vascular stain (port-wine stain), which is geographic or blotchy/segmental, dark-red, purple, or pink-red [6]. The skin discoloration is also proportionate to disease severity. Venous varicosities in the anterolateral thigh and leg are usually present at birth or in infancy due to the abnormal embryonic avalvular venous structure [7]. In childhood, the lymphatic malformation presents with chronic leakage of lymph or blood or secondary infection with pseudoverrucous hyperplasia and lymphedema, which leads to enlargement of the affected limb. The disfigurement of the genitalia can happen due to deep lymphatic malformation in the pelvis and retroperitoneal region [8]. The reasons for limb overgrowth could be multifactorial, such as soft tissue and bone overgrowth with or without vascular and lymphatic malformation [8]. There is a cohort study of 48 people in which 23 (48%) patients presented with superficial venous thrombosis, 16% (8 among 48 people) developed deep vein thrombosis and pulmonary embolism, and 2% people developed pulmonary embolism [9].
KTS is a rare and debilitating disease. Our patient developed port-wine stain, soft tissue swelling, and localized vascular malformation from birth. He also had a history of bloody discharge from skin lesions and rectal bleeding, which led to anemia and heart failure. Although the disease course is progressive, in his case, regular blood transfusion for GI bleeding is a symptomatic treatment option for several years. This is a unique case to review as the patient did not undergo any reconstructive surgery yet, however, he is maintaining his health condition with periodic blood transfusions.