Winkelwagen
U heeft geen artikelen in uw winkelwagen
The precise etiology of LA is still under debate, however, the largest known risk factor for its development remains frictional rubbing and chronic irritation of the skin. Factors such as race, sex, seasonal changes, autoimmunity, and genetic predisposition are also thought to play a role in the pathogenesis of the disease. Some believe that LA may be a consequence of the intense pruritus because the pruritus often precedes skin findings by years. 4-6
Another competing theory suggests a relationship between Epstein-Barr virus and the development of LA, but newer studies are finding the true association between these two harder to delineate. LA has also been associated with other systemic conditions, such as Sjögren syndrome, systemic lupus erythematosus, primary biliary cirrhosis, and multiple endocrine neoplasia type 2A. 3
LA is a keratinocyte-derived cutaneous amyloidosis. The amyloid deposits, which contain primarily keratin, are thought to be necrotic basal keratinocytes that have undergone conversion to amyloids after being exposed to frictional damage. 5 Histologic examination reveals eosinophilic globules in the upper dermis. 5
Epidermal findings may include hyperkeratosis and acanthosis. The amyloid deposits stained with Congo red exhibit characteristic apple-green birefringence under polarized light. 4
Erythema dyschromicum perstans (ashy dermatosis) is a distinct and somewhat controversial cutaneous eruption that may be best regarded as a form of lichen planus or lichen planus actinicus. [1, 2, 3] A consensus on terminology has been delineated. [4] Some favor a new entity, identified as acquired macular pigmentation of unknown etiology, under which the rubric erythema dyschromicum perstans, ashy dermatosis, lichen planus pigmentosus, and idiopathic eruptive macular pigmentation would fit. [5] Acquired dermal macular hyperpigmentation is an almost identical and preferable alternative umbrella term. [6]
Erythema dyschromicum perstans has a slow onset and is unlikely to resolve spontaneously. [7] The clinical course of childhood (prepubertal) may differ from that of adults, erythema dyschromicum perstans may be more likely to resolve within 2-3 years. A proposed clinical classification has been devised, dividing ashy dermatoses from erythema dyschromicum perstans with the former lacking erythematous borders, and having a third category for simulators such as lichen planus variants, and medication-induced melanodermas. [8]
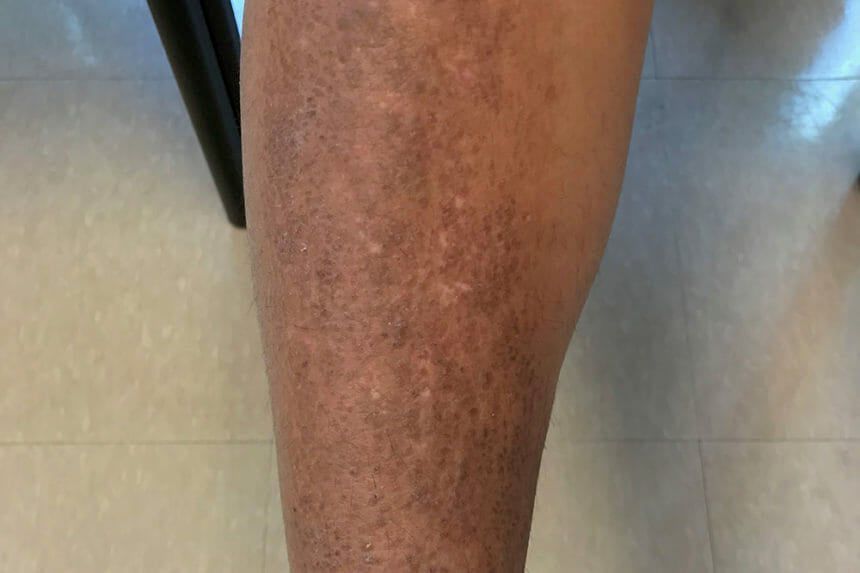
Erythema dyschromicum perstans is an asymptomatic eruption of oval, polycyclic, or irregularly shaped, gray-blue hyperpigmented macules on the trunk, the arms, the face, and the neck. It begins as ash-colored macules, sometimes with an erythematous or elevated border (see the image below). No systemic symptoms or associations exist.
Erythema dyschromicum perstans may resolve in 2-3 years in prepubertal children, but it is more likely to persist in adults. [9]
--> Ash-colored, partially confluent, macular lesions over the patient's back. Reprint with permission from Cutis 1986, 37: 42-44.
| LA | Lichen Amyloidosis |
| UVB | Ultraviolet B |
| JAK | Janus kinase |
| JAKi | Janus kinase inhibitor |
| DVT | Deep venous thrombosis |
| PE | Pulmonary embolism |
| NRS | Numeric rating scale |
| IGA | Investigator’s global assessment |
| T2IDs | Type 2 inflammatory diseases |
1. Guillet C, Steinmann S, Maul JT, Kolm I. Primary Localized Cutaneous Amyloidosis: A Retrospective Study of an Uncommon Skin Disease in the Largest Tertiary Care Center in Switzerland . Dermatology . 2022, 238 ( 3 ):579–586. doi: 10.1159/000518948 [PMC free article] [PubMed] [CrossRef] [Google Scholar]
2. Schreml S, Szeimies RM, Vogt T, Landthaler M, Schroeder J, Babilas P. Cutaneous amyloidoses and systemic amyloidoses with cutaneous involvement . Eur J Dermatol . Mar-Apr 2010, 20 ( 2 ):152–60. doi: 10.1684/ejd.2010.0842 [PubMed] [CrossRef] [Google Scholar]
3. Oetjen LK, Mack MR, Feng J, et al. Sensory Neurons Co-opt Classical Immune Signaling Pathways to Mediate Chronic Itch . Cell . Sep 21 2017, 171 ( 1 ):217–228 e13. doi: 10.1016/j.cell.2017.08.006 [PMC free article] [PubMed] [CrossRef] [Google Scholar]
Diagnosis of LA is usually based on clinical findings of the characteristic pretibial hyperkeratotic, hyperpigmented papules. The differential diagnosis for LA includes prurigo nodularis, lichen simplex chronicus, pretibial myxedema, and hypertrophic lichen planus. 2 In difficult cases, a routine skin biopsy sent for histologic examination reveals the characteristic amyloid deposits discussed above.
Patients should be told to stop scratching the lesion and to reduce friction. This can be achieved by the use of potent topical or intralesional corticosteroids that reduce pruritus and improve cosmesis. Other options include topical keratolytic agents such as salicylic acid or topical calcineurin inhibitors. 3 Patients may apply topical medications under occlusion for maximized results, occlusion serves to improve the efficacy of the topical medications and reduces frictional irritation.
In severe cases of LA, other treatment options such as dermabrasion, light therapy, and oral medications can be used. Dermabrasion has found some utility, as it allows for re-epithelialization in the damaged areas of tissue. Use of psoralen plus ultraviolet A or ultraviolet B phototherapy was shown to have moderate effects in improving pruritus and roughness in 1 study. 3 Systemic medications such as acitretin and cyclosporine have shown benefits in a small group of patients. 1
References
Wie lichen planus heeft, doet er verstandig aan voorzichtig te zijn met de huid en die zo min mogelijk te beschadigen. In de beschadigde huid kan namelijk weer een nieuwe lichen planus plek ontstaan.
Bij een uitgebreide en langdurige lichen planus aan de onderkant van de tong of op de mondbodem, bestaat er een licht verhoogd risico dat ter plekke in het slijmvlies van de mondbodem kanker ontstaat. Omdat dit risico ook wordt verhoogd door roken en alcoholgebruik, wordt geadviseerd dit te vermijden.
Sterk gekruid eten, citrusvruchten, tomaten, cafeïne-houdende dranken zoals koffie en cola, knapperig voedsel zoals toast en chips, kunnen lichen planus in de mond verergeren. Als u het gevoel heeft dat dat zo is, kunt u deze producten beter vermijden.
Lichen planus kan, indien het gepaard gaat met slechte verzorging van de mond, ook het tandvlees en het gebit aantasten. Daarom is het aan te raden om bij lichen planus van de mond regelmatig naar de tandarts of mondhygiëniste te gaan voor controle en schoonmaken van het gebit.