Winkelwagen
U heeft geen artikelen in uw winkelwagen
Omdat SLE alle organen in uw lichaam kan aantasten, is een breed scala aan klachten mogelijk die elk afzonderlijk voor kunnen komen maar vaak ook te samen. Dit zijn onder andere:
Omdat elke SLE patiënt uniek is en met een verschillende combinatie van klachten zich kan presenteren, gebruiken artsen criteria om de diagnose te bevestigen (zie tabel).
LET is extremely photosensitive, and thus sun avoidance and protection with the use of broad-spectrum sunscreens, to cover UVB and UVA spectrum, is necessary. This ideally includes sunscreens with helioplex, mexoryl, or physical blockers (titanium dioxide, zinc oxide). A sun protection factor of at least 60 should be applied daily to all sun-exposed areas. With appropriate sun protection, some LET lesions may resolve spontaneously.
Cigarette smokers are more likely to develop CLE and SLE, and to suffer from more severe disease. Patients with LET should be counseled on smoking cessation.
Overall, broad-spectrum sunscreen/sun protection and topical steroids are successful in over 50% of LET lesions. For refractory or multiple lesions, antimalarial agents are highly effective.
Antimalarials are recommended as first-line systemic therapy for CLE and SLE, given their effectiveness in prevention and treatment of symptoms such as photosensitivity, acute malar rash, discoid lupus erythematosus (DLE), oral ulcers, alopecia, arthritis, pleuritis, and pericarditis. As mentioned earlier, the vast majority of patients with LET respond to antimalarial therapy.
After 8-12 weeks, if improvement is not satisfactory, quinacrine 100mg daily may be added. Quinacrine can only be obtained at a compounding pharmacy. It may cause yellow discoloration of the skin. If the combination of hydroxychloroquine and quinacrine has not provided complete response after 2-3 months, changing to chloroquine and quinacrine is an option.
The recommended doses listed in the Table I above are based on the maximal safe dose from an ocular safety perspective. The retinopathy associated with chloroquine may be irreversible. The blurred vision and corneal deposition that may occur is reversible. The use of hydroxychloroquine necessitates eye exams every 6 months, and with chloroquine, every 4 months. The eye exam should include visual acuity, visual fields, and fundoscopic exam.
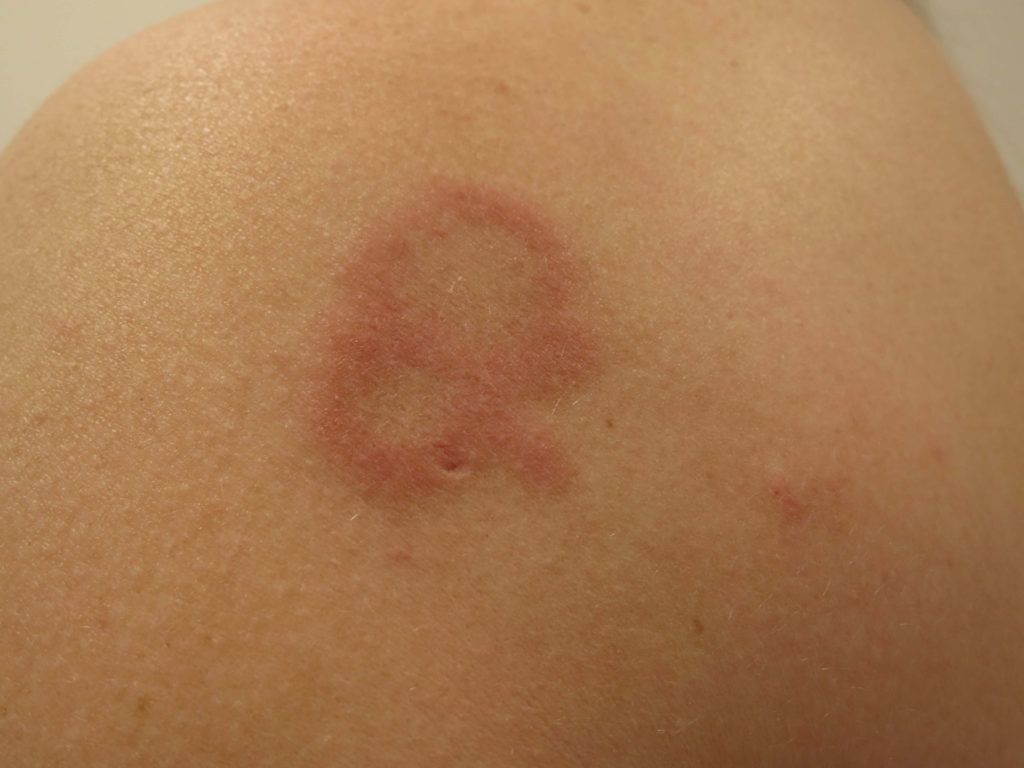
Lupus erythematosus is an inflammatory, connective-tissue disease of generalized autoimmunity characterized by pathogenic autoantibodies and immune complexes, attributed to a loss of immune tolerance. For discoid lupus erythematosus without associated SLE (CDLE), the evidence does not show whether circulating inflammatory cells and autoantibodies are involved in the pathogenesis, but it is evident that the cutaneous inflammatory infiltrates are dominated by Th1, but not Th17, cells in contrast to systemic lupus erythematosus.[5][6]
Lupus can occur in all age groups, but DLE occurs more frequently in women in their fourth and fifth decades of life. Twenty-five percent of patients with SLE may develop typical discoid lesions at some point during their illness, and 1% to 5% of patients with discoid lupus may develop SLE.
Ethnicity is also a major risk factor for developing LE, and its effect in some populations is almost as strong as that of gender. SLE prevalence is four-fold higher in African-American women than White-race American women (4 in 1000 versus 1 in 1000). In addition, African-Americans tend to develop the disease at an earlier age and have a higher mortality rate.[7][8]
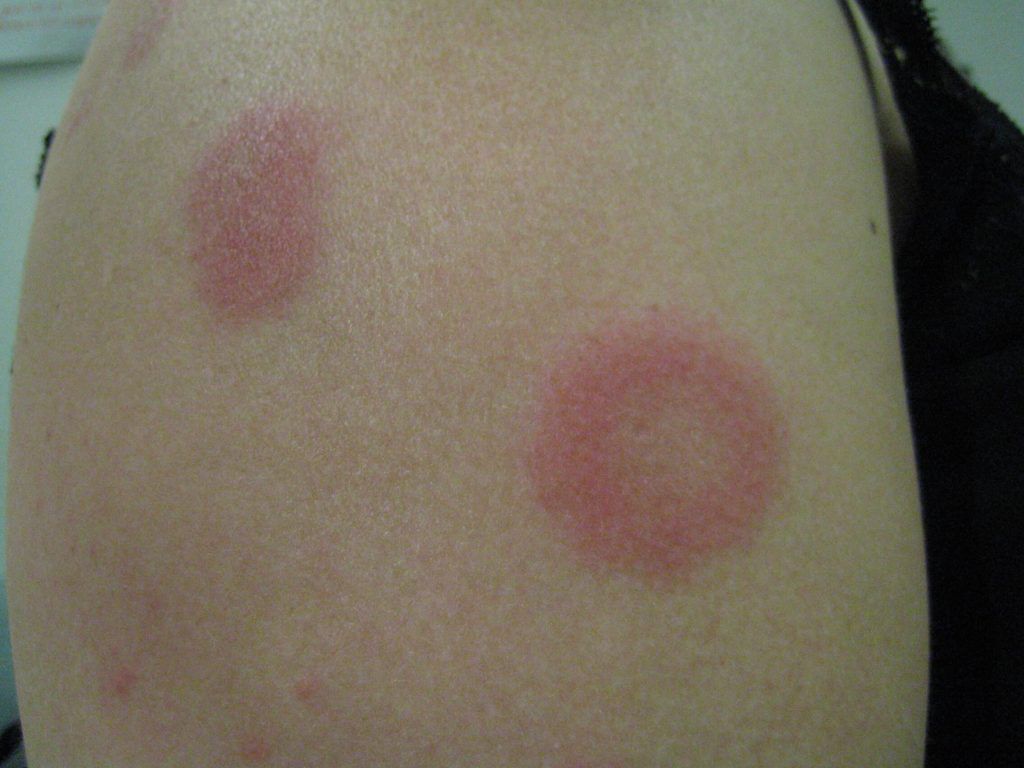
Pediatric lupus is a lifelong autoimmune condition that begins during childhood (often around age 12). Possible symptoms include fatigue, joint pain, hair loss and a “butterfly” rash on your child’s cheeks and nose. Medications can help put lupus into remission (no active symptoms) so your child can do the things they enjoy.
Lupus is an autoimmune disease that healthcare providers diagnose in people of all ages — including kids and adolescents. Providers may use the phrase “lupus in children” to refer to lupus that’s diagnosed before age 18. Although lupus generally affects children and adults in similar ways, children with lupus may have a higher risk of:
Systemic lupus erythematosus (SLE) is the most common type of lupus among children and adults. And it’s what most people mean when they talk about lupus in children. Other terms that refer to lupus in children include:
Most cases of juvenile-onset lupus start around age 12. But the disease can start sooner or later than that. It’s rare for lupus to begin before age 5.
As with any chronic condition, keeping up with treatment is essential. Your child’s healthcare team will help your family understand what treatment will involve and what to expect down the road.
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
The majority of patients have mild recurrences, usually during spring or summer, related to the first sun exposure. Educating patients on this phenomenon will help them avoid seasonal exacerbations. The majority of patients with recurrences clear with reinitiating their prior treatment regimen.
The vast majority of patients with LET have disease that primarily affects the skin. These patients should be reassured that their risk of disease progression to SLE is very low.
The next step is to provide patients with therapeutic modalities that minimize disease progression and improve treatment response. The role of smoking in disease severity and medication effectiveness must be stressed at the initial visit. All patients who smoke should be encouraged to stop smoking and should begin a smoking cessation program.
Mainstay therapies for the majority of CLE subsets, including LET, are sun protection, topical therapies, and antimalarials. These therapies have limited severe adverse reactions, however, patients with refractory or widespread disease may need therapies that carry higher side effect risks.
It is important to discuss all side effects and monitoring guidelines prior to initiating therapy. After antimalarials, there is no one agent that is superior in the treatment of LET lesions. Thus, when ascending the therapeutic ladder, individualizing therapy for each patient based on their comorbidities is necessary. Furthermore, after clearance of LET lesions, therapies should be reduced to the lowest effective dose, or discontinued.
For LET, therapies may only be needed during the spring and summer months to prevent or control disease, limiting long-term use during inactive periods of disease.
REM and lupus share many similar features, such as photosensitivity, mucin deposition, and perivascular and perifollicular lymphocytic infiltrate. Occasionally, these diseases produce a positive direct immunofluorescence. In patients with a positive ANA and other signs of LE, REM can be considered a presentation of LE. Some consider it a variant of LET.