Winkelwagen
U heeft geen artikelen in uw winkelwagen
De wratjes verdwijnen in de regel na 4 tot 12 maanden volledig. Soms blijven ze tot 2 jaar aanwezig, vooral bij kinderen met eczeem. Soms blijven kleine littekens zichtbaar. Deze littekens zijn vergelijkbaar met de littekens die na de waterpokken kunnen achterblijven.
De wratjes zelf hoeven niet per se behandeld te worden aangezien ze ook spontaan verdwijnen. In de meeste gevallen is niet behandelen en gewoon afwachten het beste. De huisarts of dermatoloog kunnen de wratjes verwijderen door middel van:
0 aanstippen met vloeibare stikstof
0 wegschrapen met een scherp lepeltje
Van tevoren kan de te behandelen huid verdoofd worden met lidocaine crème. Over het algemeen zal echter gekozen worden voor afwachten tot de wratjes spontaan verdwijnen.
gerelateerde onderwerpen
Literatuur
Forbat E et al: Molluscum Contagiosum: Review and Update on Management. Pediatr Dermatol. 2017 Sep,34(5):504-515
Molluscum contagiosum is a common medical concern. In 2010, there were about 122 million cases. It occurs worldwide but seems to be more frequent in warm, humid regions. Molluscum contagiosum is diagnosed mainly in children aged two to five years, but also in sexually active teenagers and adults, and immunocompromised persons. Atopic dermatitis may increase the risk of developing molluscum contagiosum since it alters the skin barrier and immunity function. In people living with HIV (human immunodeficiency virus), the clinical prevalence of molluscum contagiosum may reach up to 18%. No gender predominance is noted.[6]
The incubation period ranges from two weeks to six months. Molluscum contagiosum virus infects only keratinocytes, and skin lesions are limited to the epidermis and do not have systemic dissemination. Molluscum contagiosum virus produces proteins inhibiting human antiviral immunity, thus preventing the development of innate immunity response, and contributing to the persistence of skin lesions.[7]
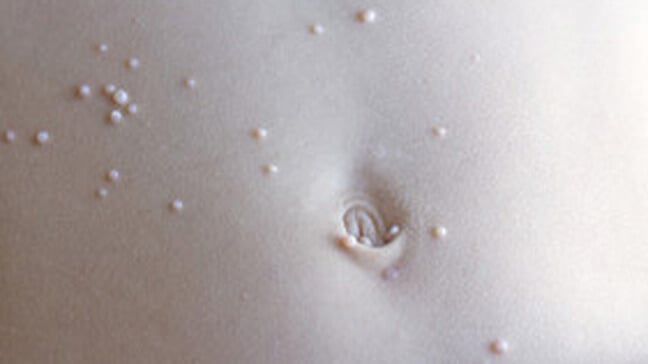
A: My favorite treatment for molluscum is nothing. Usually, kids aren’t bothered by it ― but most of the treatments are bothersome.
That said, there are several reasons (besides not knowing what the heck they are) why you might seek out help:
There’s an itchy rash around them. This reaction happens most often in kids with eczema and a topical treatment to soothe it may be needed.
Your child is self-conscious. Molluscum is most common in younger kids (preschool to early elementary), but older kids or teens can also get it and may worry about the perceived social stigma.
There are topical treatments and destructive treatments (like freezing or scraping them off, which may or may not increase the risk of scarring). There’s also some evidence that oral medications and supplements ― like the over-the-counter antacid cimetidine (Tagamet HB) and zinc ― may help the immune system fight the virus.
However, none of these treatments (though studied) are FDA-approved for molluscum. And none are wonderfully effective.