Winkelwagen
U heeft geen artikelen in uw winkelwagen
Indipendentemente dall’approccio scelto, la notalgia parestetica è una condizione che solo raramente può andare incontro ad una completa regressione, ma è comunque possibile ottenere un sufficiente controllo dei sintomi in una buona percentuale dei casi (è stato rilevato da diversi autori come la semplice spiegazione della natura benigna del disturbo consentisse un apprezzabile sollievo).
L’approccio di prima scelta consiste tipicamente nell’assunzione per via orale di gabapentin, un farmaco che nasce come antiepilettico e che tuttavia ad oggi si dimostra efficace in numerosi affezioni di tipo neuropatico.
I medicinali antistaminici, in genere l’approccio di elezione per qualsiasi forma di prurito, purtroppo non offrono alcun sollievo significativo, ma gli effetti sedativi delle molecole di prima generazione (ad esempio idrossizina, Atarax®) possono aiutare a ridurre i graffi notturni.
Tra gli approcci topici (creme, unguenti, lozioni, …) eventualmente disponibili si annoverano
In letteratura si trovano resoconti di tentativi condotti con la tossina botulinica (botulino), ma anche in questo caso i risultati sono variabili e contrastanti, come nel caso del ricorso alla TENS (apparentemente più utile in pazienti che lamentino un insieme di alterazioni della percezione, non solo prurito).
Notalgia paresthetica (NP) is a sensory neuropathy of the back, often characterized by pain. The term notalgiaparesthetica is derived from the Greek root word notos, meaning “back,” and algia, meaning “pain.” The condition was first described by Astwazaturow in 1934 and has been thought to arise from the dorsal rami of thoracic nerves T2 through T6. 1,2
Clinical symptoms of NP consist of pruritus, localized dysesthesia, and hyperesthesia in the distribution of one of the cutaneous dorsal rami of the upper thoracic region. This condition may also result in hyperpigmented skin in the scapular region. Although symptoms most often present unilaterally in the left parascapular paravertebral region, bilateral or right-sided symptoms may occur instead. In our experience, some patients complain of “tingling” and hyperalgesia with tenderness localized to the spinous processes. Sensitivity to temperature, light touch, and vibration may be abnormal, and hypoesthesia to pinprick test may be noted. 2
In the current report, we describe the case of a 59-year-old woman who presented with neck and back pain and pruritus. She was diagnosed as having NP and was treated using osteopathic manipulative treatment (OMT). A review of the literature for etiologic processes and treatment options for patients with this condition is also provided.
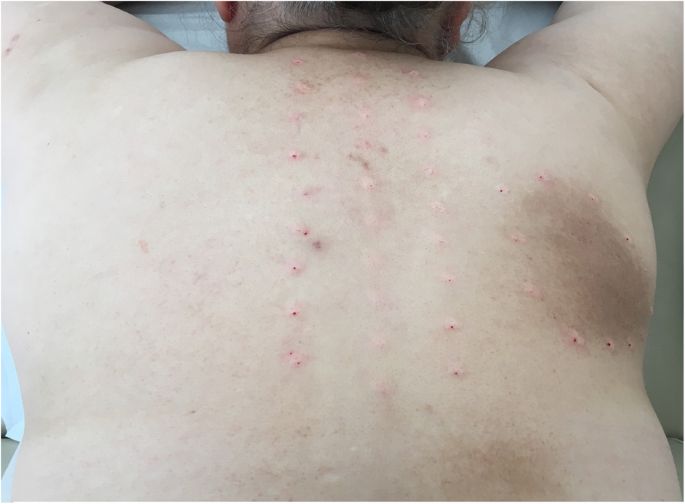
NP was first described by a Russian neurologist Astwazaturow in 1934. The term notalgia is derived from notos (back) and algos (pain). NP is a sensory neuropathy that depends on the alteration of the dorsal cutaneous sensory nerves of the upper back. This nerve alteration may be secondary to localized entrapment (possibly by the adjacent muscles) or central damage (related to the pathologies of the spine) or both [6].
Alai et al. reported a single case with cervical spinal stenosis correlated with the clinical symptoms of NP. They considered that NP might be a cutaneous sign of an underlying degenerative cervical spine disease [21]. We also observed degenerative changes and spinal stenosis mostly on the cervical spine (22%) in the NP group. The HNP of the C6–7 segment were most commonly revealed disc lesions. These findings support the idea that cervical spinal pathologies may be a contributing factor to the pathogenesis of NP.
Eisenberg et al. reported the case of a 76-year-old male with NP. His MRI revealed C4 nerve root impingement, which was associated with clinical symptoms. For the treatment of this case, the cervical epidural steroid injections applied resulted in a nearly complete recovery of symptoms [22].
Raison-Peyron et al. examined 12 NP patients with dorsal spinal X-rays and detected dorsal arthroses in nine cases. In four of six NP patients, successful results were obtained by spinal physiotherapy [15]. The relief achieved in patients through spinal physiotherapy is evidence that the pathogenesis of NP is related to the compression of the spinal nerves. In our patients, the degenerative changes and HNP of the cervical segments were more common than those of the thoracic segments. Thirty-seven cervical degenerative changes or HNP were detected in 39 patients with NP, while only nine patients had thoracic spinal lesions. According to our results, cervical spinal degenerative changes and HNPs may contribute to the pathogenesis of NP.
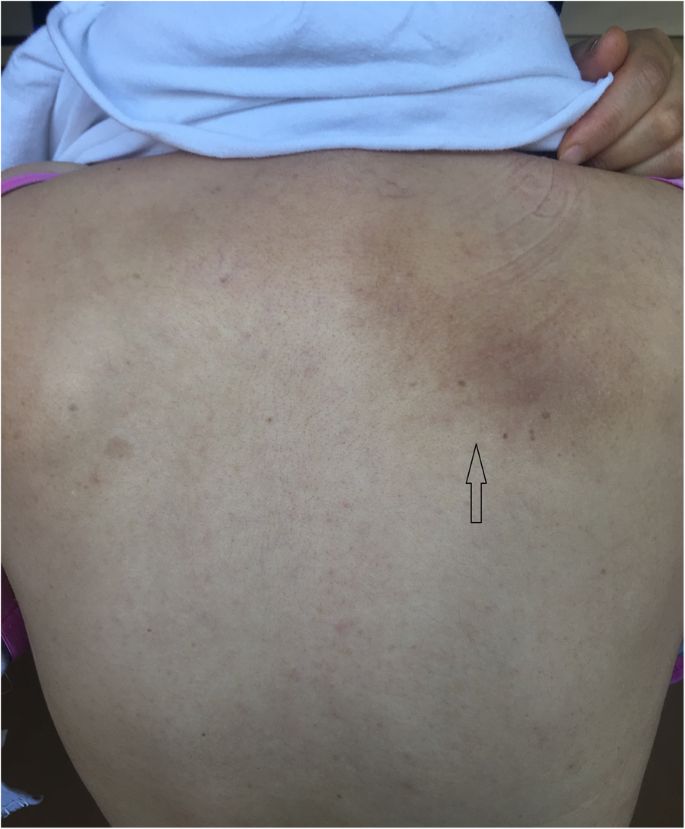
Notalgia paresthetica (NP) is characterized by localized chronic pruritus medial or inferior to the scapulae with or without an associated hyperpigmented macule. It is believed that NP is relatively common but perhaps underdiagnosed [1]. NP can exacerbate from time to time and lasts for months to years. It is widely accepted that NP is a sensory neuropathy which occurs as a result of the alteration of the cutaneous branches of the posterior rami, especially the upper branches of the T2-T6 spinal nerves [2, 3].
The arrow shows unilateral hyperpigmented macule in the medio-inferior scapulae
There are no primary cutaneous lesions in NP, these lesions are just secondary to chronic scratching and rubbing [8, 9]. Although the occurrence of NP is not rare, most cases are overlooked, therefore, it is often undiagnosed. The studies performed to date provide only limited data concerning the clinical and radiological findings of NP.