Winkelwagen
U heeft geen artikelen in uw winkelwagen
Therapeutic ladder for urticarial vasculitis.
Commonly used first-line medications in the treatment of this disease include oral antibiotics (e.g., doxycycline), colchicine (standard therapy in most neutrophilic dermatoses, including cutaneous small-vessel vasculitis), and dapsone. Hydroxychloroquine can also be used but is generally reserved for patients with co-occurring systemic lupus erythematosus. These medications have been shown to have efficacy comparable with that of corticosteroids while exhibiting fewer adverse effects and are preferable in mild cases limited to cutaneous involvement (Jachiet et al., 2018). Various nonsteroidal anti-inflammatory drugs can also be given and are especially useful for addressing musculoskeletal symptoms (Koç et al., 2017). Antihistamines fail to address the pathogenesis of this disease and as such are ineffective in most patients with urticarial vasculitis (Venzor et al., 2002). However, these medications can be added to help treat the angioedema and true urticaria lesions that occur in up to 50% of patients.
Several biologic medications have also been promising for the treatment of urticarial vasculitis and are especially useful in refractory cases when conventional avenues of therapy have been exhausted. Rituximab (anti-CD20), which is often paired with corticosteroids, hydrochloroquine, or cyclosporine, has been shown to yield higher response rates and is associated with an increased time to treatment failure when compared with corticosteroids and conventional immunosuppressives (Jachiet et al., 2018, Swaminath et al., 2011). Omalizumab (anti-IgE) is another option, and several recent case reports have supported the efficacy of this medication in the treatment of urticarial vasculitis (Cherrez-Ojeda et al., 2018, Nucera et al., 2017). Omalizumab seems to be especially effective in treating normocomplementemic patients, with investigations into its utility for hypocomplementemic urticarial vasculitis yielding inconsistent results (de Brito et al., 2018). Successful usage of this medication in conjunction with methotrexate has also been documented (Garbayo-Salmons et al., 2020). The mechanism of action of omalizumab and its role in the pathogenesis of urticarial vasculitis has yet to be elucidated and may or may not be the same mechanism by which it exerts its efficacy in the treatment of chronic urticaria (Fueyo-Casado et al., 2017).
Het is belangrijk om in de eerste fase van de aandoening rust te houden. Ook moet de huid beschermd worden tegen beschadiging omdat door de ontsteking van de bloedvaten de aangedane huid zeer kwetsbaar is geworden. Eventueel kan een beschermend verband worden aangelegd.
Met corticosteroïden (prednison) kan de ontsteking tot rust gebracht worden. Soms is een kuur van enkele dagen voldoende om het ontstekingsproces te stoppen, soms is een langere behandeling met corticosteroïden (in afbouwschema) nodig. Wanneer door de ernstige verstoring van de bloedvoorziening van de huid ter plaatse van de ecchymosen zweertjes ontstaan zal ook een goede wondverzorging moeten plaatsvinden.
In de meeste gevallen dooft de ontsteking uit en komt deze niet meer terug. Bij hardnekkige vasculitis of terugkerende episoden van ontstekingen is hernieuwd onderzoek naar de oorzaak vereist.
Gerelateerde onderwerpen
Literatuur
Lava SA et al: Cutaneous Manifestations of Small-Vessel Leukocytoclastic Vasculitides in Childhood. Clin Rev Allergy Immunol. 2017 Aug 24.
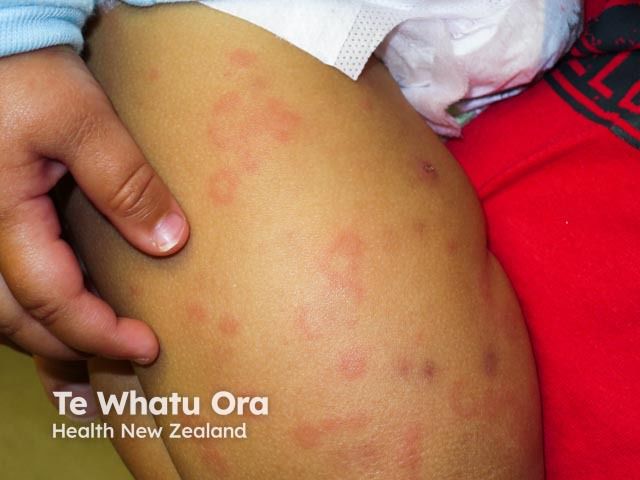
Author: Vanessa Ngan, Staff Writer, 2006. Updated by A/Prof Amanda Oakley, Dermatologist, Hamilton, New Zealand, January 2016.
Urticarial vasculitis in skin of colour
Urticarial vasculitis is generally classified as two types:
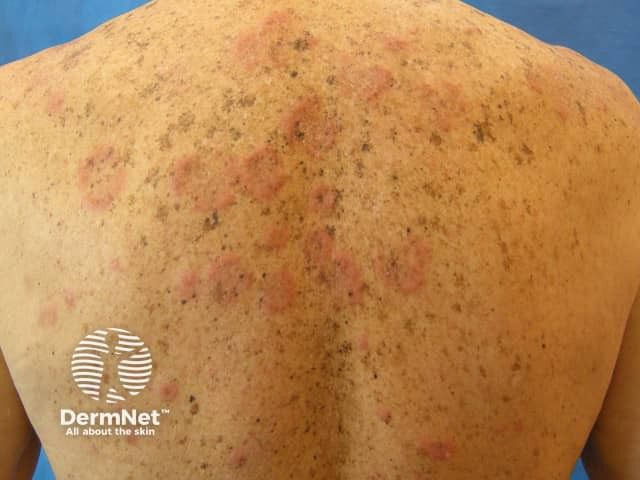
Genetic illnesses, health conditions, or infections cause your skin to react in unusual ways. Learn about these conditions and what they can do to skin.
Most of the rashes are harmless and may not indicate anything serious. However, if there are these accompanying symptoms along with the skin rash, it may signify something serious. A rash can become serious if immediate medical assistance is not provided when a patient has the below symptoms including rash covers most of the body, continuous itching, fever, and difficulty breathing
Hives are not contagious are triggered by an allergic response to a substance. Symptoms and signs of hives include a raised, itchy red rash on the skin. An individual should seek medical care for hives if he or she develops dysphagia, wheezing, shortness of breath, or throat tightening.
Hives or urticarias are red, itchy skin rashes triggered by food, medicine, or other irritants. They can vary from a few millimeters to several centimeters in diameters.
The word "rash" means an outbreak of red bumps on the body. The way people use this term, "a rash" can refer to many different skin conditions. The most common of these are scaly patches of skin and red, itchy bumps or patches all over the place.
The skin is the largest organ in the body that covers the entire external surface. It protects the internal organs from germs and thus helps prevent infections. The skin is made up of three main layers.
Could you identify a scabies infestation? Take the Skin Diseases Pictures Quiz and learn to identify common conditions that plague human skin.
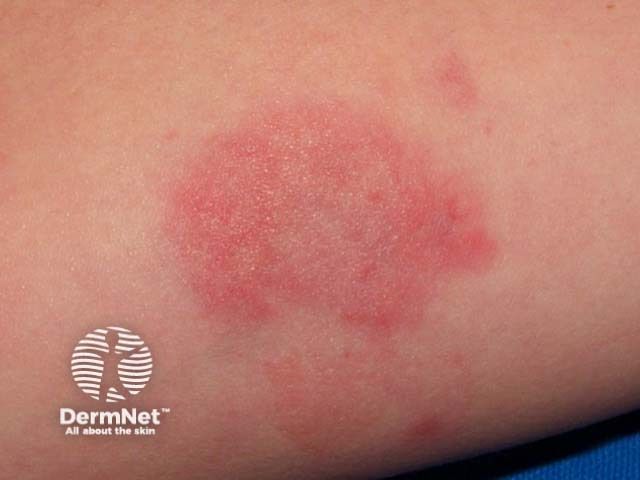
Check CH50, C3, C4, Clq, and antibodies to Clq in urticarial vasculitis patients. If these test results are positive, evaluate renal function and urinalysis to check for the effects of vasculitis on the kidneys. [22, 23, 24]
If the history suggests viral infections, obtain hepatitis B, hepatitis C, and heterophile antibody serologies.
Direct immunofluorescence may show deposition of vascular C3, fibrin, and immunoglobulins. A lupus band may be detected in patients with underlying lupus erythematosus.
If warranted, obtain antinuclear antibody and lupus serologies. Anti-SSA and anti-SSB may be seen in patients with Sjögren syndrome. Test results for antineutrophilic cytoplasmic antibodies are generally negative, and, if they are positive, the possibility of Wegener granulomatosis or microscopic polyangiitis should be considered.