Winkelwagen
U heeft geen artikelen in uw winkelwagen
Teens and adults need not stay home, but they should take the following precautions to avoid infecting others:
Dermatologists recommend treating impetigo. It can help cure the impetigo and prevent others from getting this highly contagious skin infection.
With treatment, impetigo is usually no longer contagious within 24 to 48 hours.
Without treatment, impetigo often clears on its own in two to four weeks. During this time, there is a greater risk of developing complications. You may see new blisters and sores.
It’s also possible for the infection to go deeper into the skin if you don’t treat. If this happens, you can develop ecthyma. This infection goes deeper into the skin than impetigo. As the skin heals from ecthyma, scars can form.
Ecthyma is more common in children, the elderly, and people who have diabetes. It also develops in people who are experiencing homelessness and combat soldiers fighting in a hot and humid climate.
If you see anything on your skin that looks infected, it’s best to see a board-certified dermatologist as soon as possible. An early diagnosis and treatment can prevent complications and help you feel better.
Images
Getty Images
References
Craft, N, Lee PK, et al. “Superficial cutaneous infections and pyodermas.” In: Wolff K, Goldsmith LA, et al. Fitzpatrick’s Dermatology in General Medicine (seventh edition). McGraw Hill Medical, New York, 2008: 1695-8.
Habif TP, Campbell, JL, et al. “Impetigo.” In: Dermatology DDxDeck. Mosby Elsevier, China, 2006: Card#46.
Halpern AV and Heymann WR. “Bacterial diseases.” In: Bolognia JL, et al. Dermatology. (second edition). Mosby Elsevier, Spain, 2008:1075-6.
Last updated: 3/11/21
Reproduction or republication strictly prohibited
without prior written permission.
Berikut ini adalah gejala impetigo berdasarkan jenisnya:
Impetigo krustosa merupakan jenis impetigo yang paling sering dialami oleh anak-anak dan lebih mudah menular. Gejala impetigo krustosa meliputi:
Impetigo bulosa merupakan jenis impetigo yang lebih serius. Gejalanya berupa:
Terkadang, impetigo bulosa juga disertai dengan demam dan kemunculan benjolan di sekitar leher akibat pembengkakan kelenjar getah bening.
Impetigo harus secepatnya ditangani, karena deteksi dan penanganan sejak dini dapat menghambat atau menghentikan penyebaran infeksi, serta mempercepat proses penyembuhan.
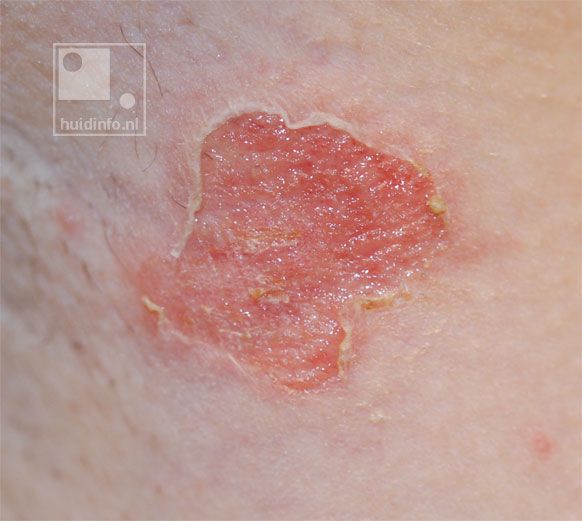
Topical antibiotics alone or in conjunction with systemic antibiotics are used to treat impetigo. Antibiotic coverage should cover both S aureus and S pyogenes (i.e. GABHS). While untreated impetigo is often self-limiting, antibiotics decrease the duration of illness and spread of lesions. In addition, antibiotic treatment decreases the chances of complications involving kidneys, joints, bones, and lungs, as well as acute rheumatic fever.[8][9][10]
For localized, uncomplicated, non-bullous impetigo, topical therapy alone is the treatment of choice. The crust should be removed with soap and water before the application of topical antibiotic therapy. Mupirocin, retapamulin, and fusidic acid are the treatments of choice.
Systemic antibiotics should be prescribed for all cases of bullous impetigo and cases of non-bullous impetigo with more than five lesions, deep tissue involvement, systemic signs of infection, lymphadenopathy or lesions in the oral cavity. Beta-lactamase-resistant antibiotics such as cephalosporins, amoxicillin-clavulanate, dicloxacillin are the treatment of choice. Cephalexin is commonly used. If culture confirms an infection solely caused by streptococci, oral penicillin is the preferred therapy.
In areas of high prevalence of MRSA or if cultures are positive for MRSA, clindamycin or doxycycline are the preferred treatments. Trimethoprim-sulfamethoxazole is effective against MRSA, but should only be used if group A streptococci are not the causative agent, or in addition to an anti-streptococcal antibiotic.
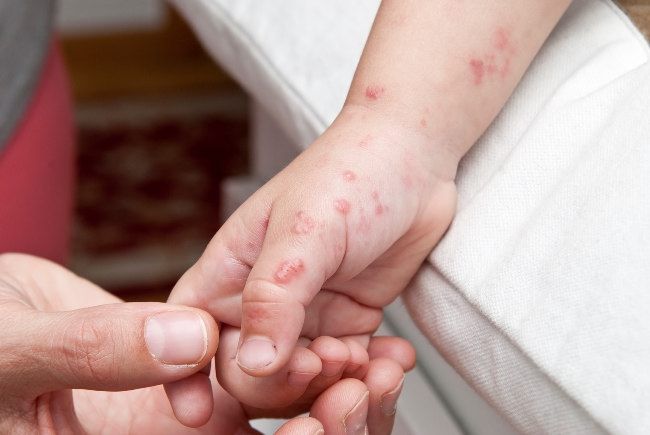
While in the past, GABHS and S aureus were equally frequent causative agents for nonbullous impetigo, currently S aureus accounts for 50-60% of cases. In developing nations and warm climates, however, GABHS is still the more common cause. [6]
Groups B, C, and G streptococci are rare causes of nonbullous impetigo. Group B streptococci are associated with impetigo in the newborn.
Coagulase-positive group II S aureus, most often phage type 71, is the predominant causative organism. This strain of bacteria produces an exfoliating toxin that causes subcorneal epidermal cleavage and the condition known as Staphylococcal scalded skin syndrome (SSSS).
MRSA has been isolated in as many as 20% of bullous impetigo cases. [6] Methicillin resistance is found on the mecA gene, which has 4 elements, I-IV. Element IV is associated with community-acquired MRSA, and elements I-III are associated with hospital-acquired MRSA.
Among the risk factors for hospital-acquired MRSA are the following:
Having a chronic indwelling catheter or medical deviceCommunity-acquired MRSA is a growing problem. Community-acquired MRSA is seen in greater frequency in closed populations in prisons, day care centers, and athletic teams, as well as in patients with diabetes or an underlying skin condition. The prevalence in these communities has been reported to be as high as 50%.