Winkelwagen
U heeft geen artikelen in uw winkelwagen
Normalerweise ist Mundsoor von einem geschulten Auge schnell zu erkennen, auf Grund seines typischen Aussehens und den weißen Belägen im Mundraum. Nichtsdestotrotz wird dein Arzt eine ausführliche körperliche Untersuchung bei dir durchführen und deine Krankengeschichte aufnehmen, da es bestimmte Faktoren gibt, die eine Erkrankung begünstigen. Beispielsweise durch inhalative Glukokortikoide, Zahnprothesen oder eine Immunsuppression, z.B. im Rahmen einer HIV-Infektion oder einer Tumorerkrankung.
Um die Diagnose zu sichern und um zu untersuchen, um welchen Erreger es sich handelt, wird dein Arzt zusätzlich eine mikrobiologische Untersuchung anordnen. Dies geschieht in der Regel durch einen Abstrich an der Mundschleimhaut. So lässt sich der Erreger identifizieren und eine adäquate Therapie einleiten.
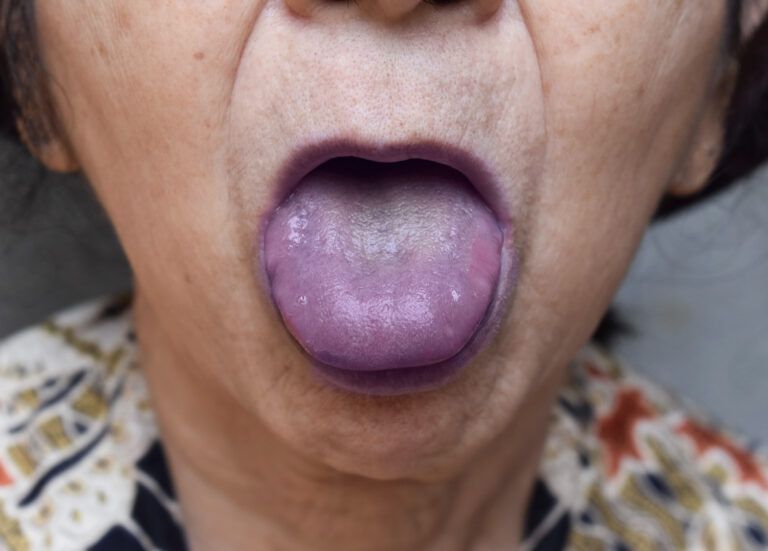
Eine Pilzinfektion im Mund kann anhand verschiedener Anzeichen und Symptome erkannt werden. Hier sind einige häufige Anzeichen, auf die du achten kannst:
1. Weiße, cremefarbene oder gelbe Flecken: Diese Flecken können auf der Zunge, den Wangen, dem Gaumen oder den Mandeln auftreten. Sie können sich ausbreiten und eine schleimige Konsistenz haben.
3. Brennen oder Schmerzen: Eine Pilzinfektion im Mund kann ein brennendes oder schmerzendes Gefühl im Mund und Rachen verursachen.
4. Schwierigkeiten beim Schlucken: Es kann schwierig sein, Nahrung zu schlucken, insbesondere wenn sich die Infektion auf den Rachen ausbreitet.
5. Unangenehmer Geschmack: Du könntest einen unangenehmen oder metallischen Geschmack im Mund haben.
6. Mundtrockenheit: Eine Pilzinfektion kann mit Mundtrockenheit einhergehen.
Es ist wichtig anzumerken, dass diese Symptome auch bei anderen Mund- oder Racheninfektionen auftreten können. Eine genaue Diagnose einer Pilzinfektion im Mund erfordert normalerweise eine ärztliche Untersuchung. Ein Arzt oder Zahnarzt kann eine visuelle Inspektion durchführen und möglicherweise einen Abstrich oder andere Tests nehmen, um den Pilzbefall zu bestätigen.
Eine Pilzinfektion im Mund, auch orale Candidiasis oder Soor genannt, wird hauptsächlich durch eine übermäßige Vermehrung des Pilzes Candida albicans verursacht. Es gibt verschiedene Faktoren, die das Risiko einer Pilzinfektion im Mund erhöhen können. Hier sind einige häufige Ursachen:
1. Schwaches Immunsystem: Ein geschwächtes Immunsystem ist einer der Hauptfaktoren, die das Risiko einer Pilzinfektion erhöhen. Dies kann aufgrund von Krankheiten wie HIV/AIDS, Diabetes, Krebs, Autoimmunerkrankungen oder aufgrund der Einnahme von Immunsuppressiva nach Organtransplantationen der Fall sein.
2. Antibiotika: Die Einnahme von Antibiotika kann das natürliche Gleichgewicht von Bakterien und Pilzen im Körper stören. Antibiotika können nützliche Bakterien abtöten, die normalerweise das Wachstum von Candida albicans kontrollieren, was zu einer Überwucherung des Pilzes führen kann.

Oral candidiasis is a clinical diagnosis. Further evaluation is necessary when a differential diagnosis is required and for cases resistant to antifungal therapy.[8] However, a biopsy is indicated for chronic hyperplastic candidiasis due to its risk of malignant transformation.[8] The commonly implemented methods for identifying Candida are 10% potassium hydroxide stain and culture with sabouraud dextrose agar.[8] Differentiation of specific species is possible with special culture mediums like Chromagar Candida.[9] ELISA and PCR tests are used in cases of invasive candidiasis and to differentiate Candida dubliniensis from Candida albicans.[8]
Pseudomembranous candidiasis, also known as oral thrush, is the classic and most common presentation of oral candidiasis, but several other types exist. Candidiasis can appear in the oral cavity as white or erythematous lesions.[3] White lesions develop as pseudomembranous or hyperplastic lesions, erythematous lesions include atrophic lesions in acute and chronic forms, angular cheilitis, median rhomboid glossitis, and linear gingival erythema.[3] Other rare oral types that cannot be included in these categories are cheilocandidiasis, chronic mucocutaneous candidiasis, and chronic multifocal candidiasis.[3]
Acute Pseudomembranous Candidiasis
Pseudomembranous candidiasis is the most frequently encountered oral candidiasis, accounting for a third of cases.[3] It is most commonly seen in newborns and immunocompromised patients,[5] but the elderly are also susceptible.[3] Other risk factors include topical steroids use in the form of inhalers, gels, or rinses and decreased salivary flow.[5]
Hyperplastic Candidiasis
Hyperplastic candidiasis presents as slightly raised and well-circumscribed white plaques, usually on the buccal mucosa, which may extend to the labial commissures.[3] The lesions may also be nodular or spotted.[3] Unlike oral thrush, hyperplastic candidiasis cannot be easily wiped off.[3] Smoking seems to be linked to the development of the lesion, and smoking cessation is required for complete resolution.[4]
