Winkelwagen
U heeft geen artikelen in uw winkelwagen
Treatment of symptomatic mild cases:
Other treatments are dependent on cause:
Severe mucosal disease:
This is a complex disease spectrum, and there is limited high quality information on the different types of adjunctive therapies and topical treatments or their desirable and undesirable effects. Considering the potential high mortality rates, the undesirable effects of the recommendation were considered less important.
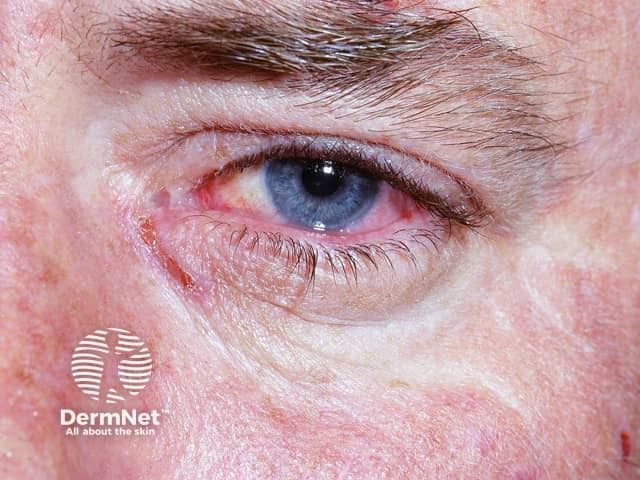
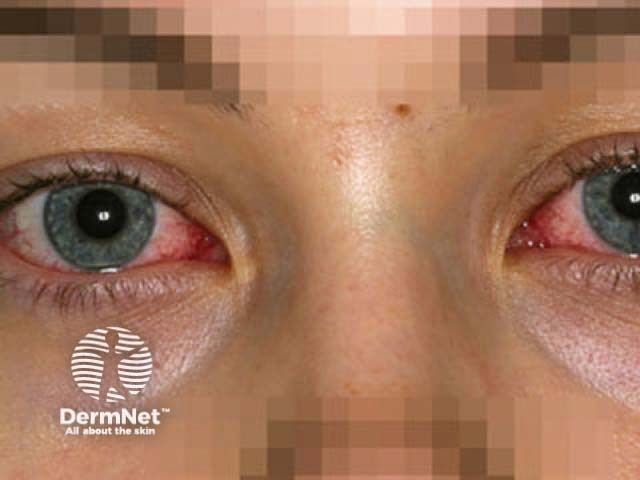
The experts agreed that early detection of SJS and toxic epidermal necrolysis is critical. Health care providers should be aware of the symptoms, including blistering, tenderness, redness, rash, erosions and photophobia.
The review did not find any good evidence to support the use of oral steroids, immunoglobulins or cyclosporine-A, all common treatments for this condition. The group considered that the use of steroids may decrease survival in the paediatric group, although the evidence was of low quality. Steroids may also place the HIV-infected patient at risk for OIs and sepsis.
Very high costs for treatment are expected, and supportive care costs are also high. It would be possible to implement the recommended approach only in larger hospitals, with good facilities for diagnosis of disease, availability of trained staff and good nursing care, and the possibility of referral. WHO’s and other recommendations on nursing burn care should be followed (WHO, 2003, Lehloenya, 2007).
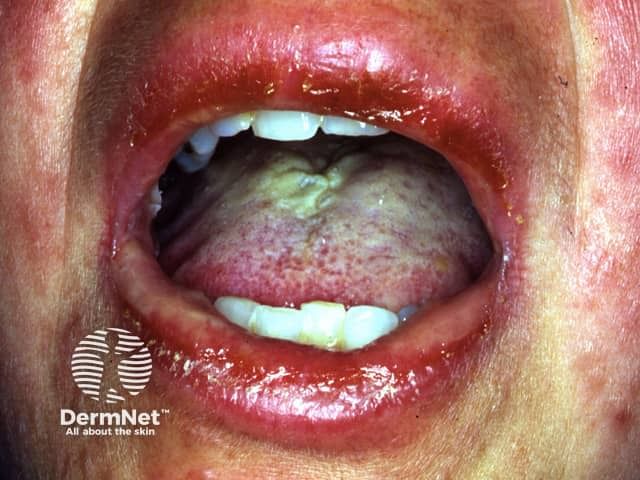
In HIV-infected children and adults with SJS or toxic epidermal necrolysis, the suspected causative drug should be promptly discontinued and supportive therapies should be offered. a
(Strong recommendation, very low quality evidence) The use of systemic corticosteroids is not recommended. (Conditional recommendation, very low quality evidence)Drugs initiated in the last one to three weeks prior to illness should be considered as potential causes and careful consideration of all drugs the patient is receiving is needed, including over-the-counter and non prescription as well as herbal and traditional medicine.
There is no reliable laboratory test to determine the offending drug, diagnosis is based on the patient’s history and the temporal relationship of suspected drugs (those initiated in the last one to three weeks prior to illness). Provocation tests are not indicated since re-exposure is likely to elicit a new episode of increased severity.
Supportive care includes intravenous fluids, environmental control, sepsis monitoring, oral antibiotics, wound dressing, dietary support, emollients and physiotherapy, monitoring for eye complications, vaginal complications, and skin-directed medical therapies including topical antibiotics, topical steroids and debridement. Sepsis monitoring, but not prophylactic antibodies, is part of this care.
These recommendations apply to HIV-negative children and adults as well.
according to WHO recommendations on nursing burn care (WHO, 2003, Lehloenya, 2007).
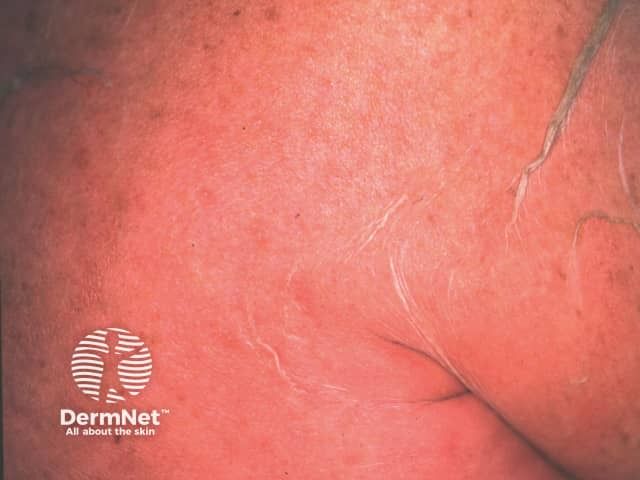
Behandeling voor het Stevens-Johnson-syndroom moet gebeuren in het ziekenhuis en begint meestal met het stoppen met het gebruik van medicatie die niet essentieel is voor de behandeling van een chronische ziekte, omdat het de symptomen van het syndroom kan veroorzaken of verergeren.
Tijdens een ziekenhuisopname kan het ook nodig zijn om serum rechtstreeks in de ader te injecteren om het vocht dat is verloren door het gebrek aan huid op de verwondingsplaatsen te vervangen. Om het risico op infectie te verminderen, moeten huidwonden bovendien dagelijks door een verpleegkundige worden behandeld.
Om het ongemak van de laesies te verminderen, kunnen koudwaterkompressen en neutrale crèmes worden gebruikt om de huid te hydrateren, evenals de inname van medicijnen die door de arts zijn beoordeeld en voorgeschreven, zoals antihistaminica, corticosteroïden of antibiotica..
Lees meer informatie over de behandeling van het Stevens-Johnson-syndroom.
Stevens-Johnson syndrome/toxic epidermal necrolysis is a rare and unpredictable reaction to medication that involves drug-specific CD8+ cytotoxic lymphocytes, the Fas-Fas ligand (FasL) pathway of apoptosis, and granule-mediated exocytosis and tumor necrosis factor-alfa (TNF–alpha)/death receptor pathway. [4][5]
Current theories address the following mechanisms, among others.
Granulysin, found in the cytotoxic granules, is the main cause of keratinocyte apoptosis.Fas–FasL, expressed on the activated cytotoxic T cells, can also destroy keratinocytes via the production of intracellular caspases.
Cytotoxic T cells exocytose perforin and granzyme B, which create channels in the target cell membrane activating the caspases.
Nitrous oxide (NO) induced by TNF–alpha and interferon (IFN)–alpha may stimulate caspases.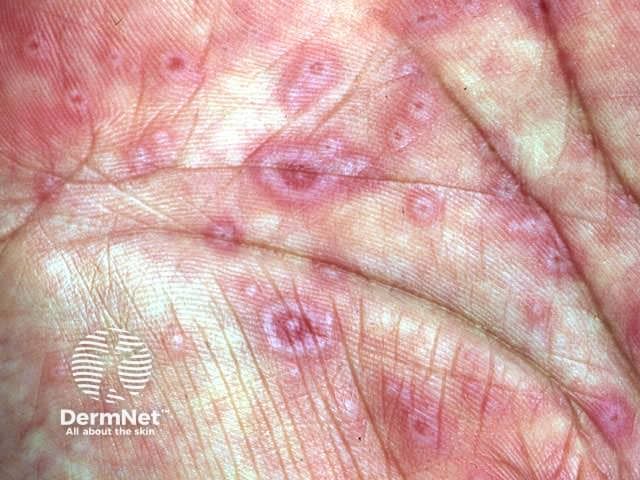
The initial step for Stevens-Johnson syndrome/toxic epidermal necrolysis may be interaction/binding of a drug-associated antigen or metabolite with the major histocompatibility complex (MHC) type 1 or cellular peptide to form an immunogenic compound. The exact mechanism is speculative.[10]
Stevens-Johnson syndrome/toxic epidermal necrolysis is T–cell-mediated.
CD8+ cells are present in blister fluid and may induce keratinocyte apoptosis. Other cells of the innate immune system play a role.CD40 ligand cells are also present and may induce the release of TNF–alpha, nitrous oxide, interleukin 8 (IL-8), and cell adhesion antibodies. TNF–alpha also induces apoptosis.
Other cells implicated in Stevens-Johnson syndrome/toxic epidermal necrolysis include macrophages, neutrophils, and natural killer (NK) cells.
The pharmacologic interaction of drugs with the immune system could result in binding of the responsible drug to MHC-1 and the T cell receptor. An alternative theory is a pro-hapten concept, in which drug metabolites become immunogenic and stimulate the immune system.