Winkelwagen
U heeft geen artikelen in uw winkelwagen
Sweet syndrome has a female predilection with a female-to-male ratio of 4 to 1. The typical age of onset is between 30 and 60 years of age, although cases have been reported in the pediatric and elderly populations as well. There has been no observed racial predilection.
The exact pathogenesis of Sweet syndrome is not known. Some genetic factors such as HLA-B54 in the Japanese population, MEFV gene mutation in familial Mediterranean fever patients, and chromosome 3q abnormalities have been observed in patients with Sweet syndrome.[9][10][11][12][10][9] Theories regarding the pathogenesis of Sweet syndrome include hypersensitivity to eliciting bacterial, viral, or tumor antigens that may trigger neutrophil activation and infiltration, leading to Sweet syndrome. Another theory suggests the role of cytokines and chemokines such as G-CSF, GM-CSF, IL-1, and interferon-gamma with a higher level of these cytokines reported in patients with Sweet syndrome.[13][14] Studies for circulating immune complexes, complement activation, and tissue bound immunoglobulins have been negative and not shown to be pathognomic in Sweet syndrome.
Ein Hautarzt könnte in der Lage sein, das Sweet-Syndrom zu diagnostizieren, indem er die Läsionen untersucht. Häufig werden aber bestimmte Tests angewandt, um Krankheiten mit ähnlichen Symptomen auszuschließen und nach der zugrunde liegenden Ursache zu suchen. So kann eine Blutprobe ans Labor geschickt werden, wo sie nach einer ungewöhnlich großen Anzahl von rote Blutkörperchen und bestimmten Erkrankungen untersucht wird.
Auch kann der Arzt eine Hautbiopsie vornehmen. Hierbei wird eine Probe des erkrankten Gewebes entnommen und unter dem Mikroskop untersucht. Das Gewebe wird dann analysiert um zu bestimmen, ob es die charakteristischen Auffälligkeiten des Sweet-Syndroms aufweist. Im Krankheitsverlauf besteht die Gefahr, dass sich die Hautläsionen infizieren.
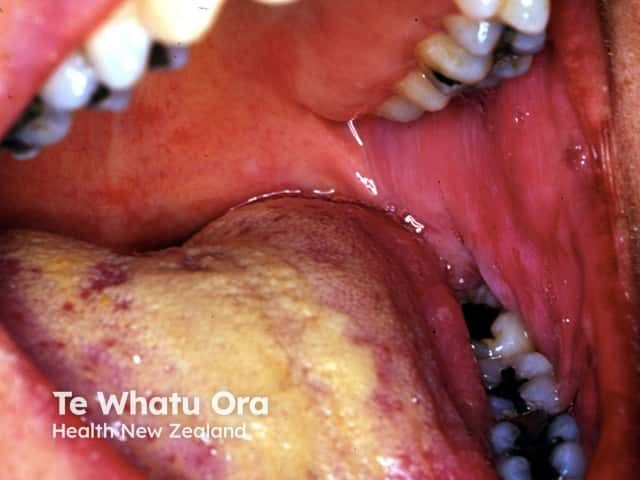
Laboratory findings in patients with Sweet syndrome include elevated markers of inflammation, including erythrocyte sedimentation rate and C-reactive protein, peripheral leukocytosis, and neutrophilia. Biopsy findings of dense can support the diagnosis of infiltrates in the superficial dermis composed primarily of polymorphonucleocytes and marked edema of the dermal papillae. Lymphocytes may also be present in the inflammatory infiltrate.
In the absence of associated malignancy or inflammatory bowel disease, Sweet syndrome is usually highly steroid-responsive and self-limiting. A 2 to 4-week tapering course of oral prednisone starting at a daily dose of 40 mg to 60 mg is usually effective. Intralesional corticosteroid injections and topical corticosteroids can also be used, especially in localized Sweet syndrome. In cases of recurrence of disease after corticosteroid tapering, several steroid-sparing agents have reportedly shown efficacy, including potassium iodide, colchicine, dapsone, isotretinoin, methotrexate, doxycycline, indomethacin, chlorambucil, and cyclosporine.[17][8][18]