Winkelwagen
U heeft geen artikelen in uw winkelwagen
Dijagnozu ove bolesti lako je postaviti i samim kliničkim pregledom zahvaćenog područja bez dlaka i noktiju.
Liječnik će Vas poslati na neke pretrage kako bi otkrili mogući uzrok alopecije (krvna slika za otkrivanje upale i anemije, jetreni enzimi za stanje jetre, temeljit pregled zubala…) Detaljan razgovor o Vašim tegobama postavit će sumnju na dodatnu bolest kao što je npr. celijakija, tireoiditis te će Vas liječnik možda poslati na pretrage koje to dokazuju (antitijela na gluten i antitiroidna antitijela).
Krvne pretrage u bolesnika s alopecijom areatom će pokazati ubrzanu sedimentaciju eritrocita.
Biopsija kože i patohistološki nalaz daju dijagnozu alopecije areate. U nalazu se vidi smanjen broj ili nedostatak folikula dlake te upalni infiltrat mononukleara, najčešće T limfocita i eozinofila. Mogu biti prisutne i promjene na žlijezdama znojnicama i lojnicama u koži. Metodom direktne imunofluorescentne tehnike vide se depoziti C3-komponente komplementa u folikulima dlake.
Untuk menegakkan diagnosis dan memastikan penyebab kerontokan rambut, perlu dilakukan pemeriksaan penunjang, seperti:
Biopsi dilakukan dengan mengambil sampel dari kulit kepala untuk diperiksa dengan bantuan mikroskop. Biopsi dilakukan untuk mendeteksi ketidaknormalan sel dan jaringan di kulit kepala serta memastikan penyebab kerontokan atau kebotakan yang dialami.
Tes ini dilakukan jika dicurigai pasien menderita penyakit autoimun atau penyakit lain yang bisa menyebabkan kebotakan dan kerontokan rambut. Beberapa hal yang akan dinilai dan dideteksi pada saat tes darah adalah:
There are multiple theories on the pathogenesis of AA. Central to these is the loss of the immune privilege of the hair follicle, leading to an attack of the follicle by the immune system. The loss of immune privilege may occur secondary to an environmental insult such as a virus, or it may be a spontaneous autoimmune phenomenon. In normal conditions, healthy anagen hair follicles express major histocompatibility complex (MHC) class I at low levels, which prevents molecular presentation as autoantigens. When this process is disturbed, and MHC expression is increased, immune privilege is lost, as previously hidden antigens may be presented to T-cells.[4]
CD8 + T-cells, in particular, are known to play a key role in the pathogenesis. These T-cells produce interferon (IFN)-gamma, which activates interleukin (IL)-2, IL-7, IL-15, and IL-21 cytokines. IL-15 suppresses regulatory T cells, promoting the proliferation of natural killer cells. Downstream, these cytokines signal the Janus kinase/ signal transducer and activator of the transcription (JAK/STAT) pathway. JAK3 is overexpressed in patients with AA.[12]

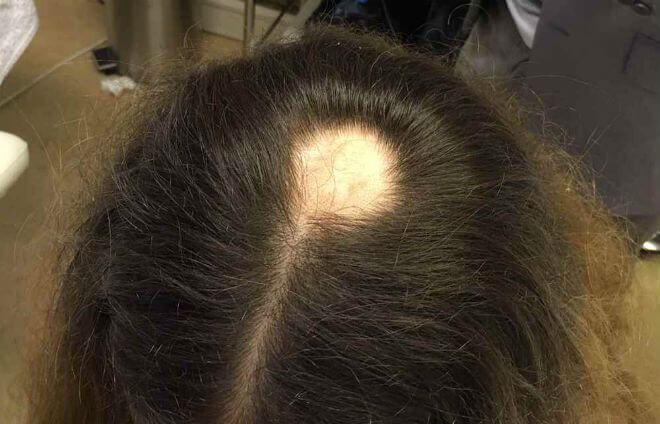
The history and physical examination are often sufficient for making the diagnosis. In most cases, the patient will have a history of patchy hair loss, which has progressed to complete loss of hair on the scalp, with the physical exam findings described above. Dermatoscopy can aid in examination. Trichoscopy, a term for dermoscopic evaluation of hair, reveals perifollicular yellow dots, black dots, tapering hairs, and vellus hairs.[16][17]
In certain patients, lab work may be indicated. Thyroid testing, such as thyroid-stimulating hormone (TSH) with reflex to free thyroxine (T4), is the most important screening laboratory test. Other tests sometimes ordered with alopecia, in general, include a complete blood count (CBC), vitamin and mineral levels, rapid plasma reagin (RPR), plasma testosterone, dehydroepiandrosterone sulfate (DHEA-S), and antinuclear antibody (ANA).
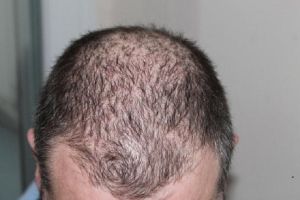
Elucidating a thorough history is critical in patients presenting with extensive hair loss. Most patients presenting with AT will have a history of discrete, patchy hair loss, which has progressed to total scalp involvement, though only 5%-10% of patients with AF progress to AT or AU.[8] For patients with AT, the most common initial presentation is multifocal AA, defined as 5 or more discrete patches. The time from the initial development of AA to progression to AT is, on average 1 year, and within 4 years in 90% of patients.[4]
Family history and past medical history are also important to obtain. There is a positive family history of hair loss in about 20% of cases. Comorbid conditions are common in patients with AA and might be slightly more frequent in those with AT, affecting about 20% of patients. Comorbidities in order of highest frequency include autoimmune thyroid disease, vitiligo, type I diabetes mellitus, atopy, and inflammatory bowel disease.[4]
On physical examination, there is a near-complete loss of scalp hair, with preservation of hair elsewhere, including the eyelashes, eyebrows, axilla, and pubic area (see Image. Alopecia Areata With Eyelash Loss). On the scalp, follicular orifices should be visible, in contrast to scarring alopecia, where they are absent. There should be minimal scalp erythema or scale. At the periphery of affected areas, exclamation point hairs may be seen. These are thick at the apex of the hair shaft and thinner towards the base of the shaft. In previously affected areas where spontaneous regrowth has occurred, the hair may initially be nonpigmented, but repigmentation usually occurs in weeks to months.
The nails should be closely evaluated as nail involvement is common in alopecia areata. This is even more frequent in patients with AT than AF and is seen in about 20%.[4] Nail pitting is the most common abnormality. Brittle nails, trachyonychia, and onycholysis are also seen.[15] See Image. Alopecia Areata Dystrophic Nails.

Iako ova bolest nije opasna i ne ugrožava život, alopecija areata ima neugodni psihološki učinak na oboljele jer uzrokuje vidljive estetske deformitete. Alopecija kod žena stvara velike neugode, srećom najčešće se javlja u akutnom i blagom obliku, a teški, kronični oblik bolesti je rjeđi. Bolju prognozu imaju bolesnici s alopecijom areatom nego bolesnici s alopecijom totalis i alopecijom univerzalis.
Alopecija areata – trajanje:
Tijek bolesti je nepredvidiv i teško je reći koji bolesnik će pripasti u koju grupu. Loša prognoza povezuje se sa sljedećim rizičnim faktorima:

